Behavioral Health Audit Risks: Planning Corrective Actions
Behavioral health organizations face increasing regulatory scrutiny, with penalties for non-compliance reaching millions of dollars.
Recent HIPAA violations, such as settlements of $225,000 and $250,000 in 2025, highlight the financial and operational risks.
Beyond fines, non-compliance can lead to license loss, denied claims, and exclusion from Medicaid or Medicare programs.
To manage audit risks, organizations can take two approaches:
Reactive: Address issues only after they arise, often leading to rushed fixes and repeated errors.
Preventive: Integrate compliance measures into daily operations, reducing errors and improving efficiency.
Key strategies include:
Conducting regular internal audits.
Using tailored EHR systems with automated compliance tools.
Standardizing documentation to meet regulatory standards.The choice between these approaches impacts costs, workflow, and risk management. While reactive methods may seem cheaper upfront, they often result in higher penalties and operational disruptions. Preventive measures, though requiring investment, help maintain compliance and avoid costly errors.
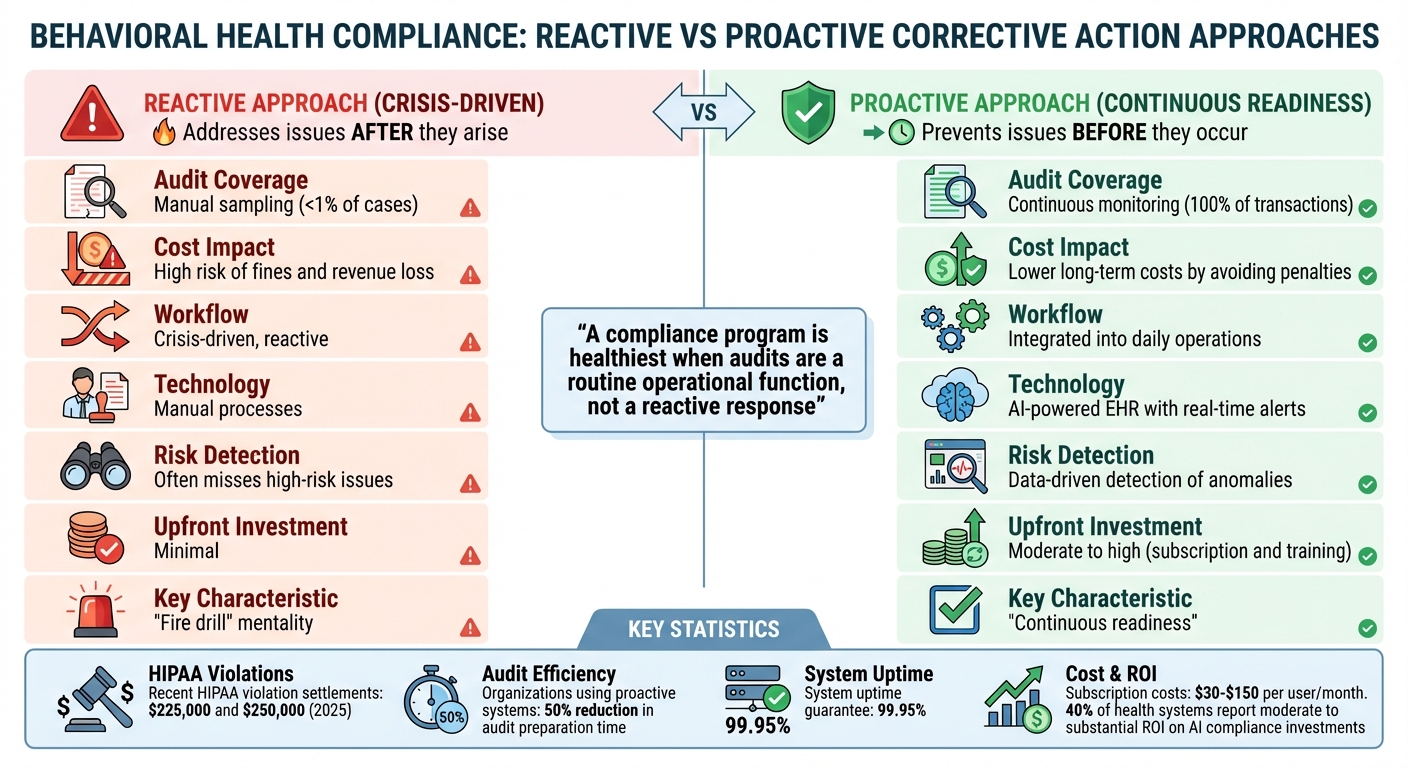
Reactive vs Proactive Compliance Strategies in Behavioral Health
A Conversation on Compliance: How Behavioral Health Organizations Can Achieve Continuous Readiness
1. Reactive Corrective Action Approaches
Reactive corrective actions kick in only after an audit trigger, such as a claim denial or a regulatory flag, has already occurred. This approach often treats compliance like a sudden emergency rather than an ongoing responsibility.
"Too often, audit readiness is treated like a fire drill; stressful, urgent, and short-lived." - John Lynch & Associates [2]
Audit Risk Mitigation
When an external auditor requests records, the immediate focus shifts to damage control. Staff scramble to retrieve records and ensure that documentation supports the billed services. Common triggers include upcoding, imprecise session times, or vague progress notes like "client discussed anxiety", which fail to specify the intervention or its impact [3].
For example, psychotherapy billing codes have strict time thresholds:
CPT 90832/90833: 16–37 minutes
CPT 90834/90836: 38–52 minutes
CPT 90837/90838: Over 53 minutes [6]If session durations are not documented accurately, claims become easy targets for denials.
A common mistake is focusing only on the flagged charts while ignoring the underlying processes that caused the issue. Conducting a root cause analysis after every audit can help identify workflow problems and prevent repeat errors [3]. It’s critical to avoid retroactively altering records in response to an audit request, as this could lead to severe legal consequences [3].
Compliance Sustainability
Reactive fixes tend to address immediate problems without implementing long-term solutions [7]. This often results in "compliance drift" between audits, where standards gradually slip [4]. Relying on manual trackers and disconnected spreadsheets adds to the burden, causing audit fatigue, staff burnout, and declining compliance quality [8].
"Compliance quality degrades not because of bad intent but because the infrastructure can't hold the load." - Alleva [8]
Instead of simply correcting flagged charts, audit findings should drive system-wide improvements. For instance, if multiple records are missing suicide risk screenings, the solution isn’t to retroactively add them but to integrate mandatory screening prompts into the intake process [3].
Operational Efficiency
Reactive responses can disrupt daily operations. When an audit notice arrives, teams are forced to pause routine tasks to retrieve records, secure signatures, and reconstruct trackers [8]. Disorganized files or delayed responses to record requests can raise red flags for auditors [3].
One way to minimize disruptions is by standardizing note templates to include essential details like date, time, duration, modality, intervention, and client response. For example, in inpatient psychiatric services, CMS requires evaluations to be completed within 60 hours of admission. Missing this deadline can lead to compliance concerns [6].
Technology Integration
In reactive models, technology is often used only for record retrieval rather than as a proactive compliance tool [1][3]. Generic electronic medical record (EMR) systems may lack features tailored to behavioral health, such as alerts for missing signatures, expired authorizations, or documentation gaps. Adopting a behavioral health–specific platform can automate these checks and reduce surprises during audits [1].
For example, platforms like Opus Behavioral Health EHR offer automated compliance tools that help organizations maintain consistent documentation standards.
|
Audit Risk Area |
Common Reactive Trigger |
Required Corrective Focus |
|---|---|---|
|
Clinical Documentation |
Missing signatures or vague notes |
|
|
Billing Integrity |
Upcoding or missing time stamps |
Accurate documentation of duration and medical necessity [3][6] |
|
Regulatory Compliance |
HIPAA/42 CFR Part 2 breaches |
|
|
Inpatient Services |
Delayed psychiatric evaluations |
Ensuring evaluations occur within 60 hours of admission [6] |
While reactive approaches can address immediate crises, they leave organizations exposed to recurring issues. These gaps highlight the need for proactive measures to ensure long-term compliance and audit readiness.
2. Proactive Corrective Action Approaches
Proactive corrective actions focus on preventing compliance issues before they arise, shifting the approach from reactive problem-solving to ongoing, integrated management. Instead of scrambling to fix problems flagged by audits, organizations embed compliance measures into daily processes, treating readiness as part of their routine operations rather than an emergency response [4].
Audit Risk Mitigation
One effective method is the dual-track audit model, which combines a yearly in-depth review aligned with regulatory standards and more frequent, focused audits targeting high-risk areas like billing accuracy and documentation completeness [4].
These smaller, internal "mini-audits" typically examine 10–20 charts, identifying vulnerabilities before external auditors - like Medicaid or other payers - step in [3]. Informal walkthroughs further prepare staff by simulating real-world scenarios, such as responding to records requests or locating supervision logs and updated policies [2].
"A compliance program is healthiest when audits are a routine operational function, not a reactive response."
– Atlantic Health Strategies [4]
Facilities that exhibit red flags - like frequent claim resubmissions, high staff turnover, or inconsistent EHR documentation - often attract greater scrutiny from auditors [2]. By addressing these risks early, organizations can reduce their exposure to audits and create a foundation for continuous compliance.
Compliance Sustainability
Proactive compliance fosters a culture of shared responsibility across clinical, billing, and administrative teams.
This approach involves creating living playbooks - centralized, searchable digital resources that outline specific roles, link to necessary forms, and include checklists for critical elements like intake forms, treatment plans, and progress notes [2][8].
To maintain compliance consistently, assign document ownership and establish a regular quality assurance schedule. This could include daily claim checks, weekly chart reviews, monthly trend analyses, and quarterly mock audits [8][4]. These structured reviews help prevent "compliance drift", where standards may slip between formal audits [4].
Operational Efficiency
Small, proactive steps like a 10–20 minute pre-billing review for each chart can significantly reduce claim denials and prevent the need for rework [8]. Using standardized templates - such as SOAP, DAP, or EMDR formats enhanced with smart prompts and dynamic picklists - streamlines documentation while ensuring it meets medical-necessity standards. This minimizes the likelihood of documentation gaps that often lead to reactive corrections [5][3].
Platforms that integrate clinical documentation with Revenue Cycle Management (RCM) systems are another key to reducing errors. These tools ensure billing codes align with documented services, cutting down on "revenue leakage." Such integration can also speed up the claim-to-payment process, reducing Days Sales Outstanding (DSO) by 5 to 7 days and improving cash flow [1][5].
|
Proactive Strategy |
Primary Benefit |
Key Tool/Action |
|---|---|---|
|
Dual-Track Auditing |
Prevents systemic errors |
Annual full review plus quarterly mini-audits [4] |
|
RCM Integration |
Reduces revenue risk |
Automated claim scrubbing & pre-authorization checks [1] |
|
Internal Walkthroughs |
Normalizes readiness |
Staff practice locating supervision logs and policies [2] |
|
AI Guardrails |
Real-time correction |
Automated flagging of missing signatures/data [1] |
Technology Integration
Advanced technology takes operational efficiency to the next level by embedding compliance tools directly into workflows.
Behavioral health EHRs equipped with AI-driven compliance features can flag issues like missing signatures, expired authorizations, or incomplete data before documentation is finalized [1].
These systems automate chart audits and recommend corrective actions on the spot, preventing minor errors from escalating into larger problems. Real-time monitoring allows for immediate intervention, eliminating the need to wait for retrospective audits [9].
Specialized platforms also help meet stringent requirements like 42 CFR Part 2, which mandates more detailed consent management than standard HIPAA rules. For providers working with substance use disorder (SUD) cases, EHRs with integrated consent tracking are essential [1].
Automated alerts further support compliance by notifying staff of upcoming deadlines or missing forms, helping to avoid costly penalties that can reach hundreds of thousands of dollars [1].
An example of this proactive approach is Opus Behavioral Health EHR, which offers AI-powered documentation tools and automated workflows tailored to behavioral health. With systems boasting 99.95% uptime [5], organizations can maintain compliance seamlessly without disrupting daily operations.
"Real audit preparedness comes from integrated systems, internal walkthroughs, and continuous staff education - not last-minute fixes."
– John Lynch & Associates [2]
Advantages and Disadvantages
When it comes to managing compliance and operational efficiency, the choice between reactive and proactive corrective action strategies can significantly shape how a behavioral health organization handles audit risks and regulatory requirements. Each approach has its strengths and weaknesses, influencing cost, workflow, and overall risk management.
Reactive strategies typically involve minimal manual sampling - less than 1% of cases[10]. While this keeps upfront costs low, it often misses high-risk areas, leaving organizations vulnerable to costly violations, such as HIPAA or 42 CFR Part 2 breaches[1].
These strategies are largely crisis-driven, addressing issues only after they arise. While this might seem cost-effective initially, the long-term risks and potential penalties can far outweigh the savings.
On the other hand, proactive strategies rely on continuous monitoring and analytics, ensuring that 100% of transactions are reviewed[10]. For instance, systems like Opus Behavioral Health EHR use AI-powered tools to flag issues like missing signatures, expired authorizations, or incomplete documentation before claims are submitted[1].
Many organizations adopt a dual-track audit model, combining annual comprehensive reviews with quarterly mini-audits of 10–20 charts[4]. While these systems require an upfront investment - subscription costs ranging from $30 to $150 per user per month, plus setup fees in the low five-figure range[5] - they often lead to measurable benefits, such as fewer penalties, faster claims processing, and improved cash flow.
Here's a quick comparison of the two approaches:
|
Dimension |
Reactive Approach |
Proactive Approach |
|---|---|---|
|
Audit Coverage |
Manual sampling (<1% of cases)[10] |
Continuous monitoring (100% of transactions)[10] |
|
Cost Impact |
High risk of fines and revenue loss[1] |
Lower long-term costs by avoiding penalties[10] |
|
Workflow Impact |
Crisis-driven, reactive |
Integrated into daily workflows[4] |
|
Technology Use |
Manual processes |
AI-powered EHR with real-time alerts[1] |
|
Risk Detection |
Often misses high-risk issues[10] |
Data-driven detection of anomalies[10] |
|
Upfront Investment |
Minimal |
Moderate to high (subscription and training)[5] |
However, proactive systems aren't without challenges. One potential risk is "transcription drift" or "autopilot errors", where staff may become overly reliant on automation, reducing their vigilance[11]. Despite this, facilities using digital solutions like Opus report up to a 50% reduction in audit preparation time, with uptime guarantees of 99.95%[5].
As one expert puts it:
"Waiting until one of these agencies uncovers a problem will likely cost significantly more than if the organization can find it and fix it beforehand"[10].
Conclusion
Taking proactive steps in compliance management creates systems that are stronger and better equipped to handle challenges than reactive approaches.
While reactive strategies may seem cheaper initially, they often lead to penalties, revenue losses, and the chaos of last-minute problem-solving. Proactive systems focus on maintaining "continuous readiness" rather than scrambling to "survive audits", which reduces stress and avoids costly fixes [8].
Reactive methods tend to address only visible problems, whereas proactive monitoring uncovers deeper, systemic vulnerabilities early on [4][8]. As Atlantic Health Strategies explains:
"A compliance program is healthiest when audits are a routine operational function, not a reactive response" [4].
The benefits of proactive, AI-driven compliance are clear. Organizations using such systems report a 70% improvement in protocol adherence, a 30% reduction in regulatory costs, and a 50% boost in operational efficiency [12].
These results highlight the importance of integrating technology and forward-thinking practices into compliance workflows.
For example, tools like Opus Behavioral Health EHR offer AI-powered features that flag issues such as missing signatures or incomplete documentation before claims are submitted [1]. Built-in field validation ensures that forms cannot be submitted unless all required information is complete, keeping records audit-ready from the start [11].
Unified dashboards also give leadership insights into clean claim rates and recurring gaps, enabling smarter decision-making [1]. These tools not only improve compliance but also streamline daily operations, setting the stage for meaningful, practical changes.
Key steps include implementing dual-track audits, standardizing documentation, and creating feedback loops to ensure continuous readiness [3][4][8]. As Alleva emphasizes:
"The real value of a well-run audit process is what happens after - using what you find to close quality gaps, strengthen workflows, and improve health care outcomes over time" [8].
Proactive compliance shifts the perspective on documentation, turning it into a tool for clinical accountability rather than just another administrative task [8].
With 40% of health systems reporting moderate to substantial returns on AI investments in compliance [12], the real question isn’t whether to adopt proactive strategies - it’s how quickly organizations can make the transition.
FAQs
What should we do first after an audit finding?
The first thing to do after receiving an audit finding is to draft and submit a detailed Plan of Correction (POC) within the required timeframe - typically 30 days. Your POC should outline the specific steps your organization has taken, or plans to take, to resolve the identified issues. This might include actions like updating policies or providing staff training. A well-prepared POC not only shows your commitment to compliance but also helps reduce the chances of similar problems happening again.
How often should we run internal mini-audits?
It's a good idea to conduct internal mini-audits on a regular basis. Many experts suggest doing these reviews at least once every quarter. Regular audits can help spot potential risks in behavioral health practices early, making it easier to address them. This approach not only ensures compliance with regulations but also supports smoother operations and improvements where needed.
What EHR features help prevent audit problems?
Opus Behavioral Health EHR offers a range of features designed to minimize audit risks. These include automated compliance workflows, which help ensure processes align with regulations, and real-time alerts to flag potential issues immediately.
The system also incorporates secure encryption to protect sensitive data, role-based access controls to limit access appropriately, and documentation templates to standardize records. Together, these tools help behavioral health providers reduce errors and maintain regulatory compliance while simplifying their workflows.
