Why Not All Behavioral Health EMR Systems Are Equal
Behavioral health practices often face unique challenges that generic EHR systems fail to address.
Here's why choosing the right EMR matters:
Efficiency: Generic EHRs add unnecessary steps, with providers spending 90 extra minutes daily on documentation.
Compliance: Behavioral health requires stricter privacy standards, like 42 CFR Part 2, which many systems overlook.
Specialized Needs: Longer sessions (45–60 minutes) and tools like DSM-5 coding and group therapy documentation are often unsupported.Outcomes: Practices using tailored systems report a 30% increase in client engagement and faster data retrieval.
Opus Behavioral Health EHR stands out by addressing these gaps with features like AI-driven documentation, built-in compliance tools, and seamless integration for billing, labs, and telehealth.
Practices using it save time, reduce errors, and improve patient outcomes. Choosing a system that aligns with your workflows can transform your practice.
Why Opus Behavioral Health EHR?
Opus Behavioral Health EHR is tailored specifically for behavioral health providers, offering a unified platform that combines clinical documentation, admissions management, and billing.
With over 160,000 practitioners using it, the system avoids generic medical templates, focusing instead on the unique needs of behavioral health workflows [6].
Usability
The Copilot AI Scribe significantly cuts down documentation time by drafting progress notes for both in-person and telehealth sessions. Providers report spending 35% less time on documentation while still capturing detailed clinical data.
For example, Dr. Jennifer Williams, a mental health practice owner, highlights the time savings and improved data accuracy [6][7]. The platform also includes over 100 customizable assessment tools - like ASAM criteria, PHQ-9, and GAD-7 - easily adaptable to different practice methodologies [6].
For residential programs, the Recovery Coaching Rounds feature allows staff to log observations and monitor patient progress across shifts directly in the EHR, eliminating the inefficiencies of paper-based systems.
Clinical Director Deborah V. shares:
The OPUS EMR system offers easy accessibility and user-friendly cross-referencing of clinical, case management, medical, and demographic data, enhancing clinical collaboration [8].
Compliance Capabilities
Opus meets rigorous compliance standards, including ONC Certification, PCI DSS Level 1, ISO 27001, FISMA Moderate, and SOC 1/SSAE 16/ISAE 3402 [9].
Security features include 2048-bit encryption for TLS communications and 256-bit encryption for session tokens using JWT with HMAC-SHA256 [9]. Multi-factor authentication (MFA) and single sign-on (SSO) add critical layers of protection, ensuring HIPAA and 42 CFR Part 2 compliance for safeguarding sensitive patient data.
Integration Options
Opus integrates admissions tracking, clinical documentation, and revenue cycle management within its unified CRM-to-RCM architecture [7].
Native lab integrations allow providers to order and receive lab results directly in the system, while DEA-compliant EPCS supports Medication-Assisted Treatment programs [7].
The platform also adheres to HL7 and FHIR interoperability standards, enabling secure data sharing with external labs, pharmacies, and other organizations. Its HIPAA-compliant telehealth module syncs session details automatically into patient records, streamlining workflows. Judd Carey, Director of Operations at VirtualServices, Mindful Health, notes:
By automating the quality of internal data, and applying an algorithm, it will cut back on errors to not miss a thing, especially from group sessions [7].
Scalability
Built on a cloud-based infrastructure, Opus supports practices of all sizes, from solo clinicians to large organizations with 36 or more providers [6].
Collectively, private practices using Opus have generated over $9.5 billion in revenue [8]. A free entry-level tier offers basic scheduling and billing features, giving practices a chance to test the platform’s core functionalities before upgrading [7].
Reporting and Outcomes
Opus includes over 140 practice management reports covering clinical, operational, and financial metrics [8].
Its outcomes measurement module tracks patient progress using standardized tools and provides visual graphs for payer and accreditation reporting [7]. These features help practices showcase treatment effectiveness and make informed decisions to improve care and resource allocation.
Advantages and Disadvantages of Behavioral Health EMR Systems
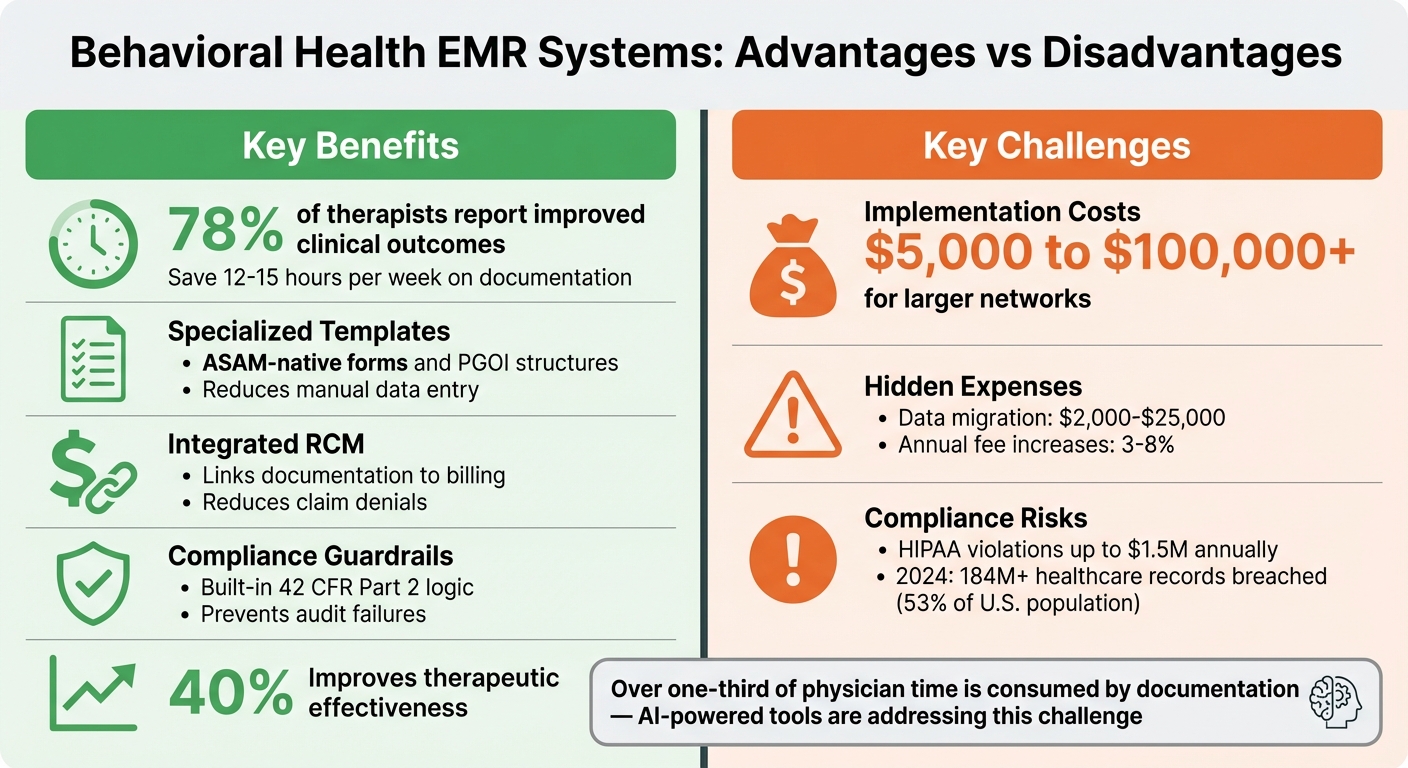
Behavioral Health EMR Systems: Advantages vs Disadvantages Comparison
Behavioral health EMR systems can save practitioners a significant amount of time, especially when tailored to mental health and addiction treatment workflows.
On average, practices using these systems save 12 to 15 hours per week on documentation, and 78% of therapists report improved clinical outcomes when using features designed specifically for behavioral health needs [10].
Tools like group notes, which allow a single note to apply to multiple clients simultaneously, eliminate hours of redundant charting [1]. Additionally, AI-powered documentation tools lighten the workload, addressing the fact that documentation typically consumes over one-third of a physician's time [2].
While these specialized features enhance efficiency, generic systems often fail to meet the unique demands of behavioral health providers.
Generic medical EHRs can create unnecessary challenges. Many lack essential features for behavioral health, such as compliance with 42 CFR Part 2 for substance use records or the ability to securely separate psychotherapy notes, as required by HIPAA. This misalignment forces providers to adapt their workflows to the software's limitations, leading to inefficiencies and added stress.
|
Advantage |
Impact |
Disadvantage |
Risk |
|---|---|---|---|
|
Specialized Templates |
ASAM-native forms and PGOI structures reduce manual data entry [1][5] |
Implementation Costs |
Fees range from $5,000 to over $100,000 for larger networks [1] |
|
Integrated RCM |
Links documentation to billing, reducing claim denials [3] |
Hidden Expenses |
Costs for data migration ($2,000–$25,000) and annual fee increases (3–8%) [1] |
|
Compliance Guardrails |
Built-in 42 CFR Part 2 logic to prevent audit failures [1][3] |
- |
- |
|
Outcome Tracking |
Improves therapeutic effectiveness by 40% [10] |
- |
- |
Compliance is another critical factor for behavioral health EMR systems. These systems must include robust safeguards, as the penalties for HIPAA violations can be severe.
For instance, willful neglect that goes uncorrected can result in fines up to $1.5 million annually [11][12]. In 2024 alone, data breaches affected 184,111,469 healthcare records - roughly 53% of the U.S. population [12][13].
To protect sensitive behavioral health information, systems should feature technical safeguards like 128-bit encryption, multi-factor authentication, and automatic audit trails. These measures are essential to maintaining data security and avoiding costly compliance issues.
How to Choose the Right EMR for Your Practice
Selecting the right EMR is a critical step in ensuring your practice runs smoothly and efficiently.
To make the best choice, the system you choose should align closely with your existing clinical workflows. A poorly matched EMR can create unnecessary obstacles, disrupting your operations. To avoid this, request demos that focus on specific workflows relevant to behavioral health.
For example, ask vendors to show how the system handles tasks like documenting group therapy, managing crisis safety plans, or processing consent for substance use disorder records.
"Investing in an EHR for your practice is more important than marketing for new clients or preparing your office space." - Kristin Trick, MA, LPC-S, RPT [4]
Before committing to a contract, clarify what the base price includes.
Tools like telehealth, e-prescribing, or integrated treatment planners often come with additional monthly fees, typically ranging from $35 to $49.
If your practice treats substance use disorders, pay close attention to compliance features. Make sure the EMR supports strong patient-level consent controls and is ONC-Certified if you bill Medicare or Medicaid. This certification ensures the system meets federal standards for security and interoperability.
Involve your entire team in the decision-making process. Non-clinical staff, like front desk or billing personnel, may notice integration issues that clinicians might miss. During demos, perform a "click count" to evaluate how many steps are needed to complete key tasks like scheduling, documentation, and billing.
A high number of clicks could signal inefficiencies that might slow down your workflow. Also, test role-based permissions to ensure sensitive therapy notes are accessible only to authorized users.
Consider the system's ability to grow with your practice. Ask whether it can handle scheduling across multiple locations, different levels of care (like IOP, PHP, or residential), and the addition of new prescribers without needing a platform switch. Get written timelines for data migration and confirm that you’ll have control over your data, including export formats, in case of future transitions.
A well-chosen EMR should support your practice’s growth, not force you to adjust your processes to fit its limitations.
FAQs
What EMR features are essential for 42 CFR Part 2 compliance?
To comply with 42 CFR Part 2, certain features are critical.
These include the ability to:
Flag SUD records to identify and handle sensitive substance use disorder information appropriately.
Manage granular patient consent, allowing patients to control who can access their records and under what circumstances.
Enforce re-disclosure restrictions to prevent unauthorized sharing of protected information.
Generate detailed disclosure audit trails to track and document all access and disclosures for accountability.
These functionalities are essential for safeguarding patient privacy while staying aligned with regulatory requirements.
How can I quickly test whether an EMR fits my workflow?
To assess if an EMR system is the right match for your practice, start by examining its core features. Look for essentials like telehealth integration, automation capabilities, real-time revenue tracking, and compliance support.
Once you've identified promising options, schedule a demo or trial. Use this opportunity to perform everyday tasks - such as documentation, billing, and patient management - to gauge how intuitive and user-friendly the system is.
This practical test helps ensure the EMR aligns with your workflow before making a commitment.
What hidden EMR costs should I ask about before signing?
Before committing, make sure to ask about any hidden costs that might come up. These could include charges for implementation support, workflow adjustments, staff training, ongoing maintenance, scaling needs, or integrations and migrations. Knowing these expenses ahead of time can save you from unexpected surprises and help you plan your budget more accurately.
