The #1 Reason People Are Choosing Behavioral Health EMR Software
Behavioral health practices are adopting specialized EMR software to address growing challenges like increased documentation time, clinician burnout, and outdated systems that don't meet their unique needs.
Here's why AI-powered documentation is transforming the field:
Time Savings: AI tools reduce documentation time by up to 40%, freeing clinicians to focus on patient care.
Improved Compliance: Tailored features ensure adherence to HIPAA and 42 CFR Part 2 regulations, minimizing risks of violations or denied claims.
Efficiency Gains: Practices report faster information retrieval, fewer errors, and streamlined workflows, leading to better financial performance.
Better Outcomes: Enhanced documentation quality translates to higher reimbursement rates and improved patient engagement.
AI-driven solutions like Opus Behavioral Health EHR are helping clinicians spend less time on paperwork and more on delivering quality care.
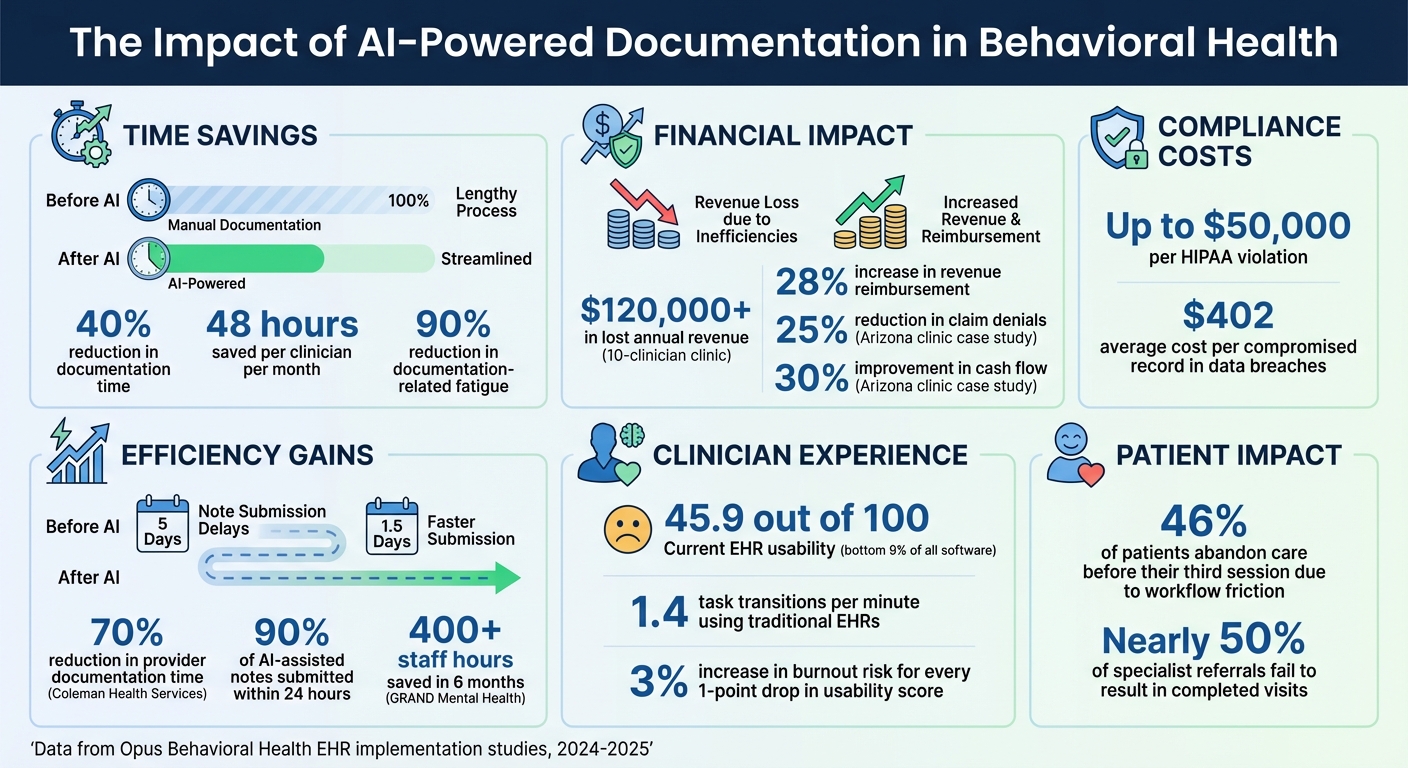
AI-Powered Documentation Impact on Behavioral Health Practices: Key Statistics
The Main Problem: Workflow Inefficiencies in Behavioral Health
Workflow inefficiencies are more than just inconveniences - they're actively draining resources and undermining the quality of care in behavioral health practices across the U.S.
At the heart of the issue are manual processes and disconnected systems, which create a ripple effect of challenges that impact care delivery, compliance, and financial stability.
Manual Processes That Slow Down Patient Care
Manual data entry alone eats up 3–5 hours of productive time every week for behavioral health providers [5].
This lost time translates into significant financial losses. For example, a mid-sized clinic with 10 clinicians could lose over 16 billable hours weekly due to documentation inefficiencies - adding up to more than $120,000 in lost annual revenue [4].
The problem doesn't stop there. Thinkitive Technologies reported that in 2025, a mid-sized behavioral health clinic lost $25,000 over a few months because of manual prior authorization tracking.
Missing renewals and letting approvals expire - due to the lack of centralized tracking systems - were key contributors to this loss [9].
Manual processes also pose safety risks. Errors from "transcription drift" - mistakes made during manual data entry - can lead to severe consequences. These include incorrect medication dosages or overlooked allergy warnings [3]. Mira Gwehn Revilla from Curogram highlights the stakes:
"A single misread digit can change a patient's life. In detox, that digit might be a medication dose. In mental health intake, it could be a suicide risk score. The stakes in behavioral health are too high for guesswork." [3]
Compliance and Documentation Requirements
Behavioral health practices face unique challenges when it comes to compliance.
They must adhere to HIPAA standards and 42 CFR Part 2, which impose stricter controls on substance use disorder records [1][7]. Unfortunately, many generic EHR systems lack the specific tools needed to meet these regulations, such as segmentation controls and consent workflows [1][7].
These inefficiencies hurt more than just productivity - they complicate compliance and increase financial risk. Inconsistent or incomplete records can trigger payer audits and lead to denied claims. Insurance companies are demanding more detailed clinical justifications, and failure to meet these standards can have costly consequences.
For instance, HIPAA violations can cost up to $50,000 per violation, while data breaches in behavioral health average $402 per compromised record in remediation costs [5].
The documentation demands are growing, too. Payers now expect detailed narratives to justify treatment decisions, but many clinicians are stuck using systems designed for simpler, checkbox-style workflows [2][7].
Effects on Clinician Productivity and Patient Care
The toll on clinicians is immense. Behavioral health providers have rated EHR usability with a median score of 45.9 out of 100, placing these systems in the bottom 9% of all software [8].
Poor usability isn't just frustrating - it directly contributes to burnout. In fact, every one-point drop in the System Usability Scale correlates with a 3% increase in burnout risk [8].
Clinicians face constant interruptions, averaging 1.4 task transitions per minute when using EHRs. This fragmented attention disrupts workflows and reduces efficiency. It's estimated that providers spend one-third to one-half of their workday interacting with these systems [8]. As John Lynch & Associates explains:
"Every minute lost to inefficient EHR workflows in behavioral health isn't just a frustration - it's a direct hit to financial stability, clinician well-being, and patient care." [4]
Patients feel the impact too. About 46% of behavioral health patients abandon care before their third session, often due to friction in scheduling and intake processes [4].
Additionally, nearly half of all specialist referrals fail to result in completed visits due to communication gaps between disconnected systems [6].
However, there is hope. In 2024, a mid-sized behavioral health clinic in Arizona partnered with John Lynch & Associates to tackle these inefficiencies.
By standardizing billing protocols and automating Revenue Cycle Management processes, the clinic achieved a 25% reduction in claim denials and a 30% improvement in cash flow within just six months [4]. This example shows that addressing workflow problems isn't just about reducing frustration - it’s about building sustainable systems that prioritize patient care.
These challenges highlight the urgent need for solutions, setting the stage for the potential of AI-powered documentation, which will be explored in the next section.
The #1 Reason: AI-Powered Documentation in Opus Behavioral Health EHR
Opus Behavioral Health EHR stands out for its Copilot AI, an advanced tool designed to tackle the inefficiencies and compliance hurdles that often overwhelm behavioral health clinicians.
How AI Changes Documentation
Copilot AI acts as a quiet yet effective clinical assistant, capturing therapy sessions in real time and automatically creating detailed, insurance-ready clinical notes [10][11][12].
Traditional documentation methods often force clinicians to choose between staying fully engaged with their patients or keeping accurate notes. This AI tool eliminates that trade-off, working seamlessly during both telehealth and in-person sessions [11].
The difference is striking. Clinicians using Copilot AI report saving an average of 48 hours each month. Additionally, 90% of users experience a noticeable drop in documentation-related fatigue [10][11][12]. Trey Wilson, CEO of Opus EHR, highlighted this breakthrough:
"In Opus EHR's quest for a genuine AI product... we recognized that we had discovered an AI solution that could genuinely cater to the needs of our clients, prospects, and clinicians" [12].
The AI-generated notes effortlessly align with pre-existing templates, ensuring compliance with payer guidelines.
This automation not only reduces transcription errors but also maintains the "Golden Thread", ensuring that assessments, treatment goals, interventions, and progress notes remain consistent and compliant [11][12][15].
By integrating so seamlessly, Copilot AI enhances efficiency while addressing the specific needs of various practices.
Customizable Workflows for Different Practice Needs
Opus Behavioral Health EHR takes these time-saving capabilities further by tailoring AI outputs to match the unique workflows of individual practices.
Clinics can customize note templates, treatment plans, and documentation formats to suit their specific focus areas, such as addiction treatment, outpatient mental health, substance use disorder programs, or integrated care.
For example, clinics dealing with substance use disorder often require detailed narrative notes, which typically reimburse around $125 per session.
On the other hand, general mental health services may benefit from streamlined progress notes, which average $70 per session [11]. The AI adapts to meet these differing needs while ensuring compliance with increasingly stringent insurance requirements.
With insurance companies now leveraging AI to audit claims for clinical justification, having accurate, well-structured notes is more important than ever [13].
Examples of AI-Powered Documentation in Practice
The real-world impact of AI-powered documentation is hard to ignore. GRAND Mental Health, a Certified Community Behavioral Health Clinic in Oklahoma, implemented this solution in January 2024.
Within six months, the clinic saved over 400 staff hours, with the AI completing more than 80% of each progress note [13].
Similarly, Coleman Health Services adopted the platform in May 2024 and saw provider documentation time drop by 70%. Burnout related to documentation decreased significantly, while note submission delays were cut from five days to just 1.5 days.
Additionally, 90% of notes assisted by AI are now submitted within 24 hours, reducing the risk of claim denials due to late filing [13][14].
The benefits go beyond time savings. Improved note quality and completeness have led to a 28% increase in revenue reimbursement [11].
Dr. Jennifer Williams, a mental health practice owner, shared her experience:
"Since implementing Opus EHR, our providers spend 35% less time on documentation while capturing more comprehensive clinical data. The AI documentation assistant feels like having an extra team member in every patient encounter" [10].
These results demonstrate how AI-powered documentation can transform practices, making it easier to manage workloads and improve outcomes. The next section will explore how to implement this system effectively.
Additional Features That Support AI Documentation in Opus Behavioral Health EHR
Opus Behavioral Health EHR doesn't just rely on Copilot AI for documentation - it brings together a range of tools in a single practice management system to enhance efficiency and accuracy.
Telehealth and E-Prescribing Capabilities
Opus Telehealth combines video conferencing, scheduling, and documentation into a single platform. This setup supports both virtual and in-person sessions, with the AI tool quietly operating in the background during consultations.
This allows clinicians to stay engaged with patients, maintaining eye contact while documentation happens seamlessly.
The integrated e-prescribing system provides instant access to AI-generated notes, diagnoses, and lab results, helping clinicians make informed medication decisions and reducing the chances of adverse drug events.
The E-Prescribe for Controlled Substances (EPCS) feature adds another layer of accuracy and security, making it especially useful for Medication-Assisted Treatment (MAT) programs. Since these systems work together, medication-related decisions are automatically added to treatment plans, eliminating the need for manual updates and ensuring a complete patient record.
Beyond virtual care, Opus enhances clinical workflows with efficient lab management tools.
Lab Integration and Reporting Options
Opus simplifies lab management by removing the need to juggle multiple systems. Lab orders and results are synchronized in real time, ensuring that orders are processed immediately and results are added to the patient’s record as soon as they’re available.
If a result is inconclusive, providers can order follow-up tests directly within the platform, speeding up the decision-making process.
Judd Carey, Director of Operations at VirtualServices, Mindful Health, highlighted the benefits:
"By automating the quality of internal data, and employing an algorithm, it will cut back on errors to not miss a thing, especially from group sessions."
To complement these features, Opus prioritizes data security and compliance.
HIPAA Compliance and Data Protection
Opus ensures top-tier security with multiple safeguards, including 2048-bit encryption for TLS protocols and 256-bit encryption for user session tokens using JWT with HMAC-SHA256.
The platform also enforces multi-factor authentication, single sign-on, and strict access controls. All patient data is encrypted, meaning Opus itself cannot access uploaded documents - data stays entirely within the customer’s control.
For substance use disorder treatments, the system supports 42 CFR Part 2 compliance through automated consent management and detailed audit trails, logging every interaction with electronic protected health information.
How to Start Using AI-Powered Documentation in Your Practice
Evaluating Your Practice's Requirements
Before diving into AI-powered documentation, gather your key team members to pinpoint where your current workflows are getting bogged down.
Take a close look at every step - patient intake, scheduling, billing - and identify areas where manual processes are slowing things down. If your practice offers specialized programs like Substance Use Disorder treatment, Mental Health services, or Foster Care support, make sure the platform you choose can handle those needs.
You'll also want to ensure compliance. Double-check that the AI tools meet HIPAA guidelines and 42 CFR Part 2 standards. Look for features like mandatory fields that prevent incomplete charts. To get a sense of the financial benefits, use an ROI calculator.
For example, Opus Copilot AI can cut clinical documentation time by up to 40% [17]. By thoroughly assessing your needs, you'll set the foundation for a smoother transition to an AI-enhanced system.
Getting Started with Opus Behavioral Health EHR
Start small by trying out the Free Complimentary User tier. This allows you to explore basic features like scheduling and billing. Once you're comfortable, schedule a personalized demo to see the full capabilities of the AI-powered documentation system in action.
This step-by-step approach helps you get a feel for the platform's interface and workflow before making a full commitment. Plus, the system offers role-based dashboards that can be customized to fit the size and needs of your practice.
Another key step is replacing paper forms with digital intake forms. These forms don’t just save time - they directly integrate patient data into the EHR. Acting as a "truth filter", they map data precisely into the system, triggering clinical alerts when high-risk responses are flagged.
This seamless integration ensures a smoother flow of information across your practice.
Getting the Most from AI-Powered Documentation
Once your workflows are running more efficiently, focus on tracking key metrics to maximize the benefits.
Train your team to use the digital intake forms effectively, ensuring they complete mandatory fields and follow timestamp protocols to maintain compliance with HIPAA and 42 CFR Part 2.
While clinicians typically adopt 80% of AI-suggested edits [13], it's crucial to encourage them to review and fine-tune these suggestions for the best outcomes.
Keep an eye on metrics like documentation time per note, how quickly notes are submitted, and staff satisfaction levels. Take Coleman Health Services as an example: in May 2024, they slashed provider documentation time by 70% and reduced note submission delays from five days to just 1.5 days, achieving a 92% satisfaction rate among their clinical team [13].
Similarly, GRAND Mental Health in Oklahoma saved over 400 staff hours in six months and cut documentation time by more than half in January 2024 [13].
As Dr. Leopoldo Pozuelo from the Cleveland Clinic puts it:
"The fact that you can have an encounter with a patient and focus on that patient with all the cognitive skills that are required of us… it's liberating."
Dr. Leopoldo Pozuelo, Center Director of Adult Behavioral Health, Cleveland Clinic
Opus Copilot AI is designed to work effortlessly on both desktop and mobile devices, requiring no extra hardware.
This makes it a great fit for both in-person and telehealth appointments. Additionally, the platform includes over 140 pre-built reports for practice management and compliance, helping you showcase improvements to stakeholders and pinpoint areas for further optimization.
Conclusion: How Opus Behavioral Health EHR Changes Behavioral Health Practices
One major draw of Opus Behavioral Health EHR is its AI-powered documentation, which has been a game-changer for behavioral health practices. By cutting documentation time by up to 40%, clinicians can save nearly 48 hours each month while reducing fatigue by an impressive 90% [11].
The platform’s unified system integrates admissions (CRM), clinical documentation (EHR), and billing (RCM) into one seamless workflow. This eliminates the need for manual data transfers, reducing errors and minimizing issues like claim denials or compliance risks.
This level of efficiency doesn’t just simplify operations - it also delivers measurable financial benefits. Insurance-ready clinical notes have helped organizations see a 28% increase in revenue reimbursement [11].
With over 160,000 practitioners using the platform and contributing to more than $9.5 billion in revenue, Opus demonstrates its value across practices of all sizes [16].
Most importantly, Opus allows clinicians to shift their focus back to what matters most: their patients.
By freeing them from excessive documentation, patient care improves significantly. The platform’s 4.8 out of 5 rating and recognition as a 2025 Software Advice FrontRunner highlight its positive impact [18]. Whether it’s a small clinic or a large residential facility, Opus ensures smoother workflows, better compliance, and improved care for patients.
FAQs
How does AI create therapy notes without hurting the session?
AI leverages natural language processing (NLP) and machine learning to transcribe and summarize sessions as they happen.
This means clinicians can concentrate entirely on their patients, while the AI takes care of documentation in the background. It does so smoothly and ethically, ensuring the flow of the session is never disrupted.
What should I check for HIPAA and 42 CFR Part 2 compliance?
When selecting a behavioral health EMR system, it’s crucial to ensure it includes the following capabilities:
Flagging SUD Records: The system should be able to identify and flag Substance Use Disorder (SUD) records to ensure they are handled with the necessary level of confidentiality.
Granular Patient Consent Management: It must allow for detailed patient consent settings, enabling precise control over who can access sensitive information.
Audit Trails of Disclosures: The system should generate clear audit trails to track any disclosures of patient information, ensuring accountability and transparency.
Re-Disclosure Restrictions: It must enforce strict re-disclosure limitations to prevent unauthorized sharing of protected information.
These features are critical for staying compliant with both HIPAA and 42 CFR Part 2 regulations, which govern the confidentiality of behavioral health and SUD records.
How can I measure ROI after switching to Opus Behavioral Health EHR?
To gauge the return on investment (ROI) of using Opus Behavioral Health EHR, focus on tracking specific metrics that reflect its impact on your practice.
Start by looking at operational improvements, such as boosted telehealth efficiency, fewer no-shows thanks to automated reminders, and reduced time spent on documentation through automation tools.
On the financial side, keep an eye on critical indicators like claim acceptance rates, denial patterns, and the average number of days accounts receivable remain outstanding.
These figures can provide a clear picture of how the system contributes to higher revenue, streamlined workflows, and better quality of care.
Together, these metrics help quantify the tangible benefits of adopting Opus Behavioral Health EHR.
