Top Features of HIPAA-Compliant Telehealth Platforms
Telehealth platforms for Substance Use Disorder (SUD) treatment must meet strict HIPAA and 42 CFR Part 2 standards to ensure patient privacy and secure sensitive data.
Key features include:
End-to-End Encryption: Protects video, audio, and messaging with advanced encryption protocols.
Secure Data Storage & Access: Includes multi-factor authentication (MFA), single sign-on (SSO), and role-based access control.
EHR Integration: Seamlessly connects telehealth sessions, billing, and patient records.
Business Associate Agreements (BAAs): Ensures compliance when sharing data with third-party vendors.
Audit Logs: Tracks all access and actions to maintain accountability.
Secure Messaging: Provides encrypted communication for patients and providers.
E-Prescribing: Allows controlled substance prescriptions with DEA-compliant security.
Consent Management: Simplifies patient consent tracking under 42 CFR Part 2.
Session Recording: Automates secure storage of session data for billing and compliance.
Platforms like Opus Behavioral Health EHR cater specifically to SUD care, integrating these features into a single system to enhance security, streamline workflows, and meet regulatory requirements.
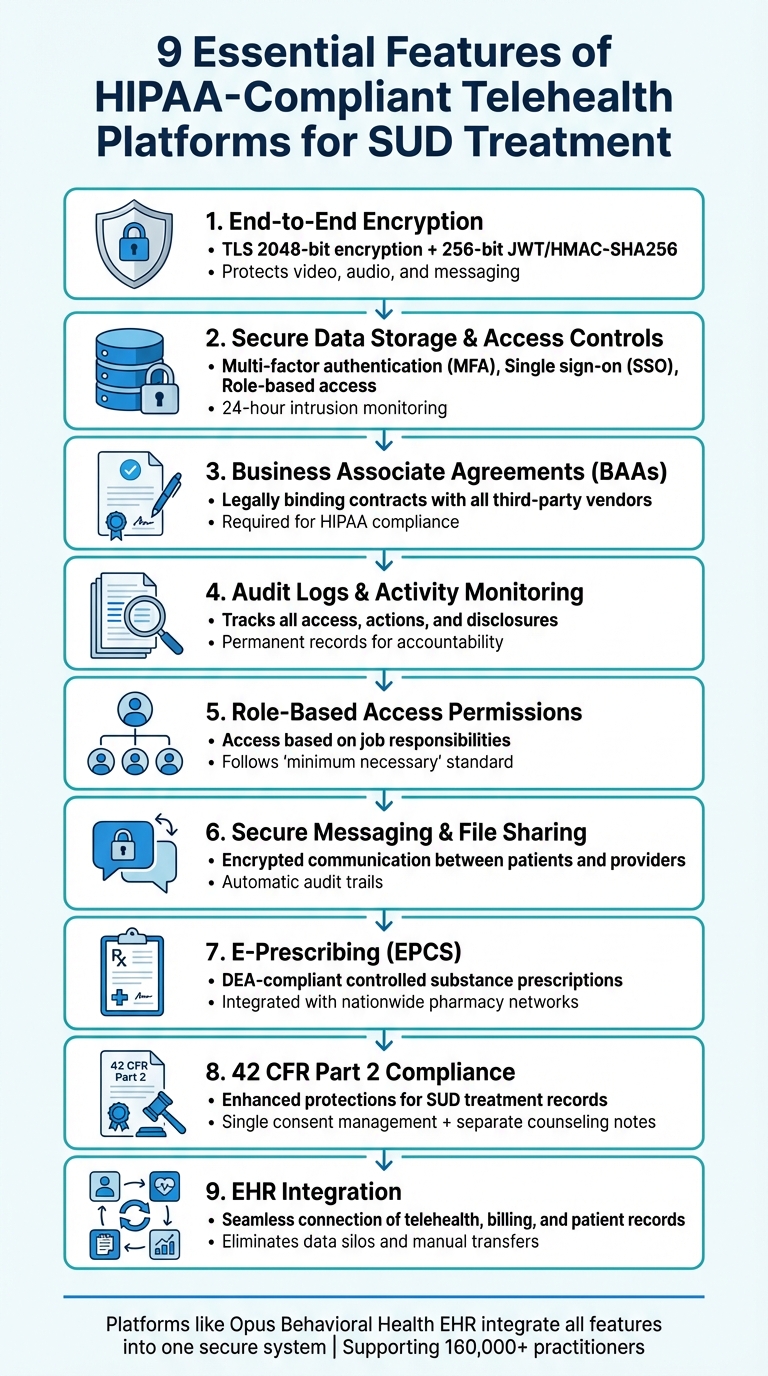
9 Essential Features of HIPAA-Compliant Telehealth Platforms for SUD Treatment
1. End-to-End Encryption for Video and Audio Sessions
HIPAA Compliance and Data Security
End-to-end encryption (E2EE) plays a critical role in securing telehealth communication, ensuring that only the sender and recipient can access the data [7]. This level of encryption protects sensitive information from hackers, unauthorized users, or even the service provider itself. To achieve this, it's essential to implement TLS with 2048-bit encryption and secure session tokens using 256-bit JWT/HMAC-SHA256 [1]. For instance, Opus Behavioral Health employs these encryption standards to safeguard patient health information during transmission and storage, fully aligning with HIPAA's Security Rule. This strong encryption framework forms the backbone of compliance efforts for telehealth platforms.
Features Supporting 42 CFR Part 2 Compliance
Substance Use Disorder (SUD) treatment records require stricter protection measures beyond what HIPAA mandates. Under 42 CFR Part 2, additional safeguards are necessary to ensure these records remain confidential [6].
"We also increased the security above HIPAA compliance standards required to care for substance abuse disorder patients." – James Schmidt, CEO, Opus Behavioral Health [5]
Encryption is vital in these cases, as it ensures that even if a platform is subpoenaed, the data remains inaccessible without the appropriate decryption keys. To further enhance compliance, confirm that your telehealth provider signs a Business Associate Agreement (BAA) [8].
Integration with Addiction and SUD Care Workflows
Secure communication is just one piece of the puzzle. Integrating telehealth solutions with Electronic Health Record (EHR) systems strengthens data protection and ensures billing accuracy. By embedding encrypted sessions directly into an EHR system, providers can avoid the risks associated with non-secure, third-party communication tools. This integration also allows session notes to be automatically stored in the patient’s permanent record while tracking session durations for precise insurance billing [5].
In October 2020, Opus Behavioral Health introduced an integrated telehealth platform that not only tracks the duration of individual and group sessions but also ensures accurate billing processes.
2. Secure Patient Data Storage and Access Controls
HIPAA Compliance and Data Security
Protecting patient data starts with robust storage protocols and strict access controls. HIPAA-compliant platforms implement measures like multi-factor authentication (MFA) and single sign-on (SSO) to ensure only authorized personnel access sensitive records [1]. Additional safeguards, such as automatic session timeouts and device detection, help prevent unauthorized access from unattended or unrecognized devices.
To further secure data, advanced systems use strong encryption for information both in transit and at rest. Administrators can also enhance security by restricting access based on factors like geographic location, IP address, or specific time windows. These features are particularly critical for safeguarding sensitive Substance Use Disorder (SUD) data [1].
Features Supporting 42 CFR Part 2 Compliance
SUD records demand heightened protection under 42 CFR Part 2, which shields the identity, diagnosis, and treatment details of patients receiving SUD care [6]. While HIPAA often allows implied consent for treatment, payment, and operations, Part 2 traditionally required explicit written consent for most disclosures [6][10].
Recent updates, such as the 2024 Final Rule, have aligned Part 2 more closely with HIPAA. Patients can now provide a single prior consent for all future uses and disclosures related to treatment, payment, and healthcare operations until they choose to revoke it [6]. Secure storage platforms play a crucial role here, managing consent records electronically and tracking exactly what can be shared and with whom. Many systems now integrate mobile signature capabilities, allowing patients to sign consent forms remotely on their devices. This not only simplifies compliance but also ensures thorough documentation [5][4].
Integration with Addiction and SUD Care Workflows
Integrating security measures within a unified EHR system enhances both compliance and data protection. By consolidating telehealth sessions, consent forms, and clinical notes into a single secure environment, providers eliminate the risks associated with using multiple disconnected platforms. This setup also supports role-based access permissions, ensuring clinicians only view data relevant to their specific patients and adhering to the "minimum necessary" standard [1].
A great example of this integration is Opus Behavioral Health, which supports over 160,000 practitioners and has facilitated care for more than 44 million clients. By unifying critical functions within one platform, Opus ensures 24-hour intrusion monitoring, threat intelligence, and firewall protection for both databases and applications. These enterprise-level security measures are tailored specifically to meet the needs of the addiction treatment industry [1][2].
3. Business Associate Agreements (BAAs) with Vendors
HIPAA Compliance and Data Security
A Business Associate Agreement (BAA) is a legally binding contract that ensures patient information remains protected when shared with third-party vendors. According to HIPAA regulations, any external service that handles protected health information (PHI) - whether it’s creating, receiving, maintaining, or transmitting it - must have a signed BAA in place before any data exchange occurs. This applies even to encrypted data and includes vendors like cloud storage providers (e.g., AWS or Google Cloud), e-prescribing platforms, and telehealth services.
The BAA outlines key responsibilities such as implementing safeguards, reporting breaches, and terminating agreements if HIPAA terms are violated. Without a properly executed BAA, organizations risk facing severe financial penalties.
"The purpose of a Business Associate Agreement is to close this enforcement loophole. Under §164.504(e), covered entities are required to ensure business associates do not engage in 'patterns of activity' that may be in violation of HIPAA."
– HIPAA Journal [11]
Features Supporting 42 CFR Part 2 Compliance
For substance use disorder (SUD) care providers, BAAs play an even more critical role. Updates in February 2024 aligned 42 CFR Part 2 with HIPAA, allowing business associates to redisclose Part 2 records under the HIPAA Privacy Rule. As a result, telehealth vendors’ BAAs should explicitly address how SUD records are handled. This includes provisions for managing "SUD counseling notes" and implementing the updated single consent workflow for treatment, payment, and healthcare operations.
Providers must ensure their BAAs include specific requirements under 42 CFR Part 2, such as:
Breach notification protocols
Restrictions on using records in legal proceedings without patient consent
Maintenance of audit trails for all PHI disclosures [12]
While a signed BAA is essential, it doesn’t automatically ensure compliance. Providers should conduct audits of their vendors to verify HIPAA risk assessments, review policies, and confirm that PHI is only handled by services explicitly covered under the BAA. These tailored agreements are especially crucial when working with specialized telehealth platforms designed to meet the unique compliance needs of SUD care.
Integration with Addiction and SUD Care Workflows
For addiction treatment centers, telehealth platforms built specifically for SUD care can provide BAAs that align with the sector’s unique requirements. For example, in October 2020, Opus Behavioral Health EHR introduced a telehealth platform tailored to SUD facilities. This platform integrates seamlessly with its electronic health record system, addressing the specific demands of addiction treatment workflows.
"Unlike Zoom or other mainstream video conferencing tools, the new Opus Telehealth platform is the only technology that is made specific to the SUD vertical and offers comprehensive tracking of patient time on individual and group sessions, which is a must-have for these centers to bill properly."
– James Schmidt, CEO of Opus Behavioral Health [5]
4. Audit Logs and Activity Monitoring
HIPAA Compliance and Data Security
Audit logs play a crucial role in maintaining data security by permanently recording who accessed patient information, when they accessed it, and what actions they performed. This level of transparency helps healthcare facilities quickly detect unauthorized access and respond to potential security breaches. Many advanced systems now incorporate 24-hour intrusion monitoring and threat intelligence tools to protect sensitive data [1]. These platforms also monitor staff usage patterns and client reporting activities, ensuring compliance and accountability [9].
HIPAA-compliant cloud recording features add another layer of functionality. They allow clinical supervisors to review therapy sessions, annotate recordings for training purposes, and maintain detailed records. These records not only support audits but also contribute to improving patient safety and outcomes [14].
Integration with Addiction and SUD Care Workflows
Detailed audit logs do more than protect data - they also enhance operational efficiency. For substance use disorder (SUD) treatment centers, accurate tracking of session durations is vital for proper billing. In October 2020, Opus Behavioral Health introduced a telehealth platform designed specifically for SUD care, seamlessly integrating with electronic health records (EHR). CEO James Schmidt highlighted its importance:
"The new Opus Telehealth platform is the only technology that is made specific to the SUD vertical and offers comprehensive tracking of patient time on individual and group sessions, which is a must-have for these centers to bill properly to health insurance companies." [5]
Automated data quality reviews further improve efficiency by reducing documentation errors in group sessions. Judd Carey, Director of Operations at VirtualServices, Mindful Health, explained:
"By automating the quality of internal data, and applying an algorithm, it will cut back on errors to not miss a thing, especially from group sessions." [2]
These tools not only ensure compliance but also support care teams in monitoring patient progress, moods, and behaviors. This real-time tracking enables timely interventions, reducing the risk of crises or relapses [14].
Features Supporting 42 CFR Part 2 Compliance
SUD records require heightened privacy measures due to their sensitive nature. Audit trails are essential for documenting all access to protected health information (PHI) and any disclosures made. These logs capture details about SUD-specific consent and enforce access restrictions based on factors like location, IP address, and time [1][5][12].
Additionally, audit systems must differentiate "SUD Counseling Notes" from general medical records. These notes require separate consent for disclosure, ensuring compliance with privacy regulations [12]. This level of granular monitoring allows facilities to provide patients with a clear record of disclosures, as mandated by HIPAA and the CARES Act [6].
5. Role-Based Access Permissions
HIPAA Compliance and Data Security
Role-Based Access Control (RBAC) ensures that Protected Health Information (PHI) is only accessible to users based on their job responsibilities. For example, clinicians, billing staff, and administrators are given varying levels of access, adhering to HIPAA’s "minimum necessary" standard. This approach minimizes unnecessary exposure to sensitive data. Advanced platforms take it a step further by restricting access based on factors like location, IP address, and time of access. They also secure communications using robust encryption methods, such as 2048-bit TLS and 256-bit session tokens, providing an additional layer of protection [1]. This structured access system also seamlessly incorporates the extra safeguards required for handling Substance Use Disorder (SUD) records.
Features Supporting 42 CFR Part 2 Compliance
SUD records demand stricter privacy measures than standard HIPAA regulations. With RBAC, sensitive information like "SUD counseling notes" can be isolated from general medical records, ensuring that only the clinician who authored them has access. This level of control is essential for maintaining patient privacy. Additionally, the 2024 Final Rule, issued by the U.S. Department of Health and Human Services on February 8, 2024, brought SUD protections closer to HIPAA standards while preserving the confidentiality critical for SUD patients [6][12].
Scalability and Integration with Existing Systems
RBAC not only enhances security but also supports scalability. By leveraging secure data storage and detailed audit logs, it ensures that every team member can access only the information necessary for their role. This scalability allows treatment centers to grow without compromising security or incurring extra costs for non-clinical staff like schedulers or billing personnel. Each user is assigned unique credentials, which enforce role-specific access and reduce the risks associated with shared logins [1].
6. Secure Messaging and File Sharing
HIPAA Compliance and Data Security
Secure messaging and file sharing tools must adhere to the same stringent standards as video sessions when protecting patient communications. Encryption plays a critical role here - platforms need to implement strong encryption protocols comparable to those used in secure video calls [1]. Unlike standard email or SMS, which fail to meet HIPAA requirements, dedicated secure messaging systems ensure all patient communications are encrypted and logged within the platform. This setup prevents Protected Health Information (PHI) from unintentionally leaking into personal devices or unsecured channels, while also creating an automatic audit trail for every message sent or received [8]. Such encryption-based systems integrate seamlessly with clinical workflows, enhancing both security and functionality.
Integration with Addiction and SUD Care Workflows
HIPAA-compliant, two-way encrypted chat functions - similar in appearance to SMS - allow patients to reach out between sessions for support or clarification. This continuous connection is especially valuable in Substance Use Disorder (SUD) care, where maintaining communication and addressing concerns promptly can significantly improve treatment outcomes [13][8]. Features like mobile signature capabilities simplify collecting patient consent directly within these secure communications, expediting enrollment processes for SUD programs [5][4]. Andrea Baskin, Clinical Director, emphasized the impact of these tools:
"The ability to run groups online has enabled us to create a digital IOP program, with flexible after hours for our clients. We don't have to worry about transportation logistics, office hours, or staff availability." [4]
Broadcast messaging adds another layer of functionality, enabling providers to send targeted updates - such as notifying therapy groups about schedule changes [13]. Additionally, EHR-integrated file sharing ensures that important documents like lab results and educational materials are automatically recorded in the patient's central record [8]. These measures ensure that regulatory compliance extends beyond basic data security.
Features Supporting 42 CFR Part 2 Compliance
SUD records require stricter confidentiality protections compared to standard HIPAA regulations. Secure messaging platforms must support features like single prior consent management, where a single signed document from the patient covers all future uses and disclosures for treatment, payment, and healthcare operations [6][10]. In October 2020, Opus Behavioral Health introduced a telehealth platform designed specifically for SUD care, exceeding standard HIPAA requirements by incorporating enhanced security measures tailored to this patient population [5].
Platforms must also include redisclosure protections, which notify recipients that SUD records cannot be shared without explicit patient consent or a court order [6]. These safeguards are critical for upholding the confidentiality of sensitive patient information.
Scalability and Ease of Integration with Existing Systems
Secure messaging platforms should offer seamless integration with EHR systems, enabling bidirectional data flow so that patient updates and files are accessible across clinical departments without the need to switch between systems [13]. Message logging further supports clinical documentation and simplifies insurance reimbursement by providing a complete record of provider-patient interactions [8]. Providers can also set communication boundaries, such as "no-reply" hours on weekends, to maintain professional standards while still offering between-session support [8].
With over 160,000 practitioners utilizing integrated EHR and telehealth platforms, unified systems that combine secure messaging, scheduling, and documentation streamline operations and reduce administrative burdens [2][4]. These tools not only simplify workflows but also ensure that telehealth remains focused on delivering safe, efficient, and compliant care.
7. E-Prescribing Integration for Controlled Substances
HIPAA Compliance and Data Security
E-prescribing for controlled substances (EPCS) demands stricter security measures than standard telehealth practices. According to DEA guidelines, only authorized providers are allowed to prescribe controlled substances [15]. To meet these requirements, platforms use advanced security protocols like 2048-bit TLS encryption for secure transmission and 256-bit HMAC-SHA256 to safeguard session tokens [1]. These measures help prevent unauthorized access and reduce fraud risks that can arise with traditional paper prescriptions.
To further enhance security, platforms implement organization-wide multi-factor authentication (MFA) and single sign-on (SSO). Additional safeguards, such as 24-hour intrusion monitoring and IP-based access controls, ensure that only verified clinicians can access prescribing tools [1]. These robust protections address the unique risks of prescribing controlled substances and support seamless integration into clinical workflows.
Integration with Addiction and SUD Care Workflows
E-prescribing systems integrated with electronic health records (EHR) streamline workflows for clinicians managing addiction and substance use disorder (SUD) care. These systems provide instant access to clinical notes, diagnoses, lab results, and patient history, reducing the chance of errors during Medication-Assisted Treatment (MAT) programs [15]. Prescriptions are sent electronically to nationwide pharmacy networks, eliminating the need for manual calls or faxes and improving medication adherence.
As Opus Behavioral Health explains, "DEA guidelines allow for use of E-Prescribe for controlled substances, adding an extra level of protection for your MAT programs" [15]. Additionally, interaction checks built into EHR systems enhance patient safety by flagging potential medication conflicts during MAT.
Scalability and Ease of Integration with Existing Systems
Integrated platforms that combine e-prescribing, EHR, and telehealth offer a comprehensive view of patient care, eliminating the need to switch between systems [13]. This seamless data sharing enables SUD treatment centers to expand geographically, supporting remote prescribing and easing transitions from residential to outpatient care without being tied to specific locations [15][4]. With over 160,000 practitioners already using these platforms, the operational benefits are clear [2].
When selecting a platform, ensure it is specifically approved for EPCS, as not all systems meet federal security standards for controlled substances [15]. Features like single sign-on simplify secure access to integrated data, streamlining processes from patient intake to billing. This not only enhances clinical safety but also supports operational growth [13].
8. Compliance with 42 CFR Part 2 Regulations
Features Supporting 42 CFR Part 2 Compliance
The 42 CFR Part 2 regulations provide more stringent confidentiality protections than HIPAA when it comes to substance use disorder (SUD) treatment records. These rules cover sensitive information such as patient identity, diagnosis, prognosis, and treatment details [6]. The goal is to reduce the stigma and fear of discrimination or prosecution, which can discourage individuals from seeking the help they need for addiction treatment [6]. This regulatory framework has a significant impact on how telehealth services are structured for addiction care.
To comply, telehealth platforms must include mobile signature tools that allow patients to provide direct consent, addressing the explicit consent requirements [5]. Recent updates to the regulations now allow a single consent to cover all future uses for treatment, payment, and healthcare operations (TPO). This change simplifies processes while respecting the patient’s rights [6][12]. Additionally, platforms must ensure the ability to separate SUD counseling notes, which are detailed clinician records requiring distinct consent for disclosure [12].
"42 CFR Part 2 is a vital element of regulatory compliance for telehealth providers, emphasizing the confidentiality of SUD patient records." - Marlene M. Maheu, PhD, Telehealth.org [12]
Integration with Addiction and SUD Care Workflows
In October 2020, Opus Behavioral Health introduced a telehealth platform tailored specifically for addiction treatment providers. This platform integrates seamlessly with their electronic health record (EHR) system, enabling detailed tracking of patient time during both individual and group therapy sessions - an important feature for accurate billing and compliance [5].
The platform also includes audit logs that automatically document every instance of access, use, or disclosure of protected SUD information. This level of tracking is essential because 42 CFR Part 2 places strict limits on how SUD records can be used, particularly in legal, civil, administrative, or legislative proceedings. Access to such records requires either explicit patient consent or a court order [6][12].
9. Automated Session Recording and Consent Management
HIPAA Compliance and Data Security
Session recordings are safeguarded with advanced encryption methods, including 2048-bit TLS and 256-bit JWT encryption, ensuring both live communications and stored files remain secure [1]. To further protect sensitive information, recordings are encrypted at rest, making them unreadable in the event of unauthorized access.
Additional security measures include robust access controls such as multi-factor authentication (MFA), single sign-on (SSO), and automatic session timeouts, all designed to prevent unauthorized access to recorded protected health information (PHI) [1]. Some platforms go even further by allowing access restrictions based on geographic location, IP addresses, or specific time windows [1]. These security protocols integrate seamlessly into telehealth workflows, offering both convenience and peace of mind.
Integration with Addiction and SUD Care Workflows
Automated recording systems do more than just document sessions - they also track therapy durations, ensuring accurate billing for Substance Use Disorder (SUD) care [5]. For example, in October 2020, Opus Behavioral Health launched a telehealth platform tailored specifically to SUD treatment. This platform integrates directly with electronic health record (EHR) systems, addressing a critical need in the industry. CEO James Schmidt highlighted its key advantages:
"Unlike Zoom or other mainstream video conferencing tools, the new Opus Telehealth platform is the only technology that is made specific to the SUD vertical and offers comprehensive tracking of patient time on individual and group sessions, which is a must-have for these centers to bill properly to health insurance companies." [5]
The platform also introduced a mobile signature engine that allows patients to review and sign consent forms directly on their smartphones. Once signed, these forms are automatically uploaded to the patient’s EHR file, streamlining workflows and eliminating delays [4][5]. Additionally, AI-powered scribe tools generate progress notes from session recordings, reducing manual input errors and maintaining clinical accuracy [2][5]. Today, over 160,000 practitioners rely on the Opus platform to manage these essential workflows [2].
Features Supporting 42 CFR Part 2 Compliance
In addition to secure recording, automated consent management ensures compliance with 42 CFR Part 2 by accurately documenting every disclosure. Recent updates to the regulations now allow a single consent for future treatment, payment, and healthcare operations (TPO). However, counseling notes for SUD treatment still require separate, specific patient consent [12]. Each disclosure must either include a copy of the consent form or clearly outline the scope of the consent provided [12].
Automated workflows and audit logs play a crucial role in maintaining compliance. These logs are particularly important since 42 CFR Part 2 imposes strict limitations on how SUD records can be used in legal or administrative proceedings without explicit patient consent or a court order [12]. By automating these processes, platforms help organizations meet these stringent requirements with ease.
Scalability and Ease of Integration with Existing Systems
As behavioral health practices expand into multi-location operations, their telehealth platforms must scale efficiently to handle increasing session data without compromising performance. Unified systems that combine video conferencing, scheduling, documentation, and consent management - while seamlessly integrating with EHR systems - help eliminate data silos and reduce the risk of HIPAA violations during manual file transfers [4][5].
For instance, in 2024, Care Counseling Clinics adopted the Opus EHR and Telehealth platform to support their growth. Trevor Mulvey, VP of Finance at Care Counseling Clinics, explained that as their organization expanded, they needed a reliable partner capable of scaling alongside them. The platform provided advanced features for back-office support, payor rate compliance, and accrual accounting reporting, ensuring their clinical and financial workflows remained synchronized throughout the expansion [2]. This scalability makes the system an ideal choice for multi-location facilities [2].
10. Integration with EHR and Billing Systems (e.g., Opus Behavioral Health EHR)
HIPAA Compliance and Data Security
When EHR and billing systems are directly integrated, it removes the risks associated with juggling multiple third-party apps. Everything - video conferencing, scheduling, and documentation - stays within a single, secure, HIPAA-compliant environment. Industry-standard encryption protocols safeguard all electronic transmissions, ensuring patient data remains protected [1].
These integrated systems also give you full control over your data. Unlike some platforms, they don’t scan your documents or emails for unrelated purposes. All uploaded content is encrypted and remains inaccessible to the vendor [1]. On top of that, security measures like multi-factor authentication (MFA), single sign-on (SSO), and IP address restrictions provide extra layers of protection. These features align with compliance standards such as PCI DSS Level 1, ISO 27001, FISMA Moderate, and SOC 1/SSAE 16 [1]. This seamless integration keeps patient data connected across both clinical and billing workflows.
Integration with Addiction and SUD Care Workflows
For substance use disorder (SUD) treatment, generic video conferencing tools don’t cut it. Platforms designed specifically for SUD care offer features like detailed session tracking, which are critical for accurate insurance billing and effective care management [5]. A great example is Opus Behavioral Health's telehealth platform, launched in October 2020, which was tailored specifically for SUD care.
This platform also includes a mobile signature feature, allowing patients to receive and sign consent forms directly on their smartphones. Once signed, the forms are automatically uploaded to the EHR, streamlining the process [4][5]. The system has proven it can handle the demands of high-volume SUD workflows [2].
Scalability and Ease of Integration with Existing Systems
Integrated platforms not only enhance security and workflows but also scale effortlessly as your practice grows. This scalability ensures compliance and eliminates data silos, providing real-time, two-way data flow between CRM and EHR systems [13]. By automating these processes, manual data entry is reduced, which minimizes the risk of errors and potential security breaches.
In 2024, Mindful Health implemented Opus EHR across multiple treatment centers, significantly improving workflows. Judd Carey, Director of Operations, highlighted the benefits:
"By automating the quality of internal data, and applying an algorithm, it will cut back on errors to not miss a thing, especially from group sessions." [2]
The platform also offers robust reporting tools, enabling data-driven decisions to enhance operational efficiency [2].
How Can HIPAA Compliant Telehealth Platforms Prevent Fines? - Telehealth Care Expert
Conclusion
Choosing the right telehealth platform is a crucial step in ensuring compliance, patient safety, and operational efficiency in SUD care. With regulatory shifts like the end of HIPAA enforcement discretion in August 2023, the alignment of 42 CFR Part 2 with HIPAA in February 2024, and the DEA's extended telemedicine prescribing flexibilities through December 31, 2025, it's clear that platforms must keep pace with evolving requirements without disrupting daily workflows [18][17]. These changes highlight the importance of using a platform tailored specifically to the needs of behavioral health.
Generic telehealth tools often fail to meet the unique demands of SUD care. Platforms designed for SUD, such as Opus Behavioral Health EHR, offer critical features like comprehensive session tracking that supports accurate billing and improved patient care [5]. Built-in compliance tools streamline workflows, reducing the risk of manual errors and enhancing overall efficiency.
When evaluating telehealth platforms, prioritize features like end-to-end encryption, audit logs, role-based access controls, and 42 CFR Part 2 consent management. Ensure the vendor is willing to sign a BAA and conducts regular security risk assessments covering all telehealth workflows [16][18]. Most importantly, opt for a solution that integrates video conferencing, scheduling, and documentation into a single, HIPAA-compliant system.
Platforms like Opus Behavioral Health EHR provide this unified approach, supporting over 160,000 practitioners and serving more than 44 million clients while exceeding basic HIPAA security requirements [2][3]. By choosing a platform built specifically for SUD care, you can meet the rigorous demands of compliance, enhance operational efficiency, and prioritize patient protection.
FAQs
What features make a telehealth platform HIPAA-compliant for SUD care?
A telehealth platform designed for substance use disorder (SUD) care must ensure it meets HIPAA requirements to safeguard sensitive patient data. Essential features include end-to-end encryption to protect data during transfer and storage, multi-factor authentication to limit access to authorized users only, and secure HTTPS connections for all communication. The platform should also maintain audit-ready logs and implement privacy measures specifically addressing the unique needs of SUD care.
By following these guidelines, providers can securely deliver telehealth services, uphold patient confidentiality, and stay compliant with regulatory standards.
How does EHR integration improve telehealth for addiction treatment?
EHR integration plays a key role in making telehealth sessions more effective and efficient. With this setup, clinicians can securely access and update patient records, schedule appointments, document visits, and handle billing - all without leaving the platform. By centralizing these tasks, it not only boosts workflow efficiency but also ensures continuity of care while safeguarding patient privacy.
In addiction treatment, real-time access to detailed patient data becomes especially valuable. It enables clinicians to make informed decisions and offer care that’s tailored to each individual. Beyond simplifying administrative tasks, this integration allows providers to focus more on delivering high-quality care during telehealth sessions.
Why are Business Associate Agreements important for HIPAA-compliant telehealth platforms?
Business Associate Agreements (BAAs) play a key role in maintaining HIPAA compliance for telehealth platforms. These agreements legally bind telehealth providers to protect protected health information (PHI), clearly define security obligations, and outline procedures for handling data breaches.
By setting clear expectations, BAAs help protect patient information, ensure adherence to HIPAA privacy and security standards, and minimize legal risks for healthcare providers utilizing these platforms.
