Behavioral Health Reporting: Key Metrics to Track
Behavioral Health Reporting: Key Metrics to Track
Behavioral health care is shifting toward data-driven practices to improve patient outcomes and meet regulatory demands.
Historically reliant on subjective evaluations, the field is now embracing tools like the PHQ-9 and GAD-7 to measure progress and adjust treatments effectively.
Key takeaways include:
Patient-Reported Outcome Measures (PROMs): Tools like PHQ-9 (depression) and GAD-7 (anxiety) provide measurable insights into symptoms and functionality.
Outcome vs. Process Metrics: Only 21% of current quality measures focus on outcomes, highlighting a need for more patient-centered reporting.
EHR Integration: Automated systems streamline data collection, offering real-time insights and reducing administrative workload.
Value-Based Care Alignment: Frequent assessments and longitudinal tracking support reimbursement models tied to measurable improvements.
Best Practices in Addressing Behavioral Health Outcomes: Measuring Care for Success
1. Patient-Reported Outcome Measures (PROMs)
PROMs are tools designed to quantify patients' symptoms, daily functioning, and overall quality of life. By standardizing this data, they transform behavioral health care from subjective observations into measurable insights that guide treatment. Common examples include the PHQ-9 for depression, GAD-7 for anxiety, PCL-5 for PTSD, and C-SSRS for suicide risk. These measures help clinicians track how patients feel over time, offering a reliable foundation for informed decision-making [3][5].
Patient Outcomes Tracking
PROMs are particularly effective in evaluating symptom severity, functional abilities (like performing daily tasks), and health-related quality of life. They also monitor behaviors such as substance use and medication adherence [4]. For instance, in August 2024, Dr. Suzette Glasner, Chief Scientific Officer at Pelago, shared that patients with alcohol use disorder achieved a 68% daily abstinence rate after 12 weeks of treatment - an impressive jump from the 10-15% observed at intake [6]. Similarly, Boulder Care's Chief Operating Officer, Rose Bromka, highlighted that payer data showed a 40% to 70% reduction in emergency room visits and inpatient stays among Medicaid members [6].
"When we're looking at how to use data to improve patient outcomes and to inform patient care, it's important to think about it as a measurement-based care model so you're actually doing something with the data that you gather that directly impacts the course of treatment." - Dr. Suzette Glasner, Chief Scientific Officer, Pelago [6]
These measures pave the way for integrating data into clinical workflows, ensuring that patient care is both responsive and evidence-based.
Data Integration and Reporting
EHR systems now play a key role in automating PROM processes. Patients can complete assessments through digital forms or portals before their appointments, which not only saves time but often results in more candid responses [5][7]. The system then calculates scores and interprets results using validated benchmarks, offering clinicians immediate decision-making support [5][7]. For example, Recovery Centers of America revamped their clinical approach under Dr. Pete Vernig, Vice President of Mental Health Services, by using data to assign patients to tailored care pathways based on their initial assessments [6].
Longitudinal Analysis
The real strength of PROMs lies in their ability to track patient progress over time. EHR systems can generate visual trends, allowing clinicians to spot improvements or potential relapses at a glance [5][6]. Conducting assessments annually, like with the PHQ-9, often falls short of providing actionable insights [1]. Instead, increasing the frequency of evaluations during critical treatment periods delivers real-time data that supports timely adjustments. Studies show that this approach improves retention, reduces no-shows, and enhances clinical outcomes [1]. Additionally, this ongoing tracking aligns with value-based payment models, where reimbursement is tied to measurable patient progress rather than the volume of services provided [3][6].
2. Opus Behavioral Health EHR
Patient Outcomes Tracking
Opus Behavioral Health EHR includes an Outcome Measurement Tool (OMT) that allows treatment centers to monitor patient engagement and treatment success with flexibility [2]. By incorporating clinical scales like PHQ-9 and GAD-7, it captures essential patient symptom data. It also tracks non-clinical metrics such as Average Length of Stay and patient satisfaction [3]. To evaluate client loyalty, the platform uses the Net Promoter Score (NPS), which ranges from –100 to 100; scores between 70 and 100 are considered top-tier [3].
Andrea Horwitz, Clinical Director, shared:
"Reviewing weekly treatment results shows me what is really happening with my clients, even if they are not able to express it in session." [2]
These metrics integrate seamlessly with larger data systems, enabling real-time reporting and providing a clearer picture of patient progress.
Data Integration and Reporting
Opus Behavioral Health EHR combines CRM, EHR, and RCM functionalities into a single platform. This integration simplifies communication across departments and eliminates the need for third-party tools [8][9]. The system offers access to over 140 practice management reports and more than 100 customizable assessment tools, allowing organizations to create tailored dashboards and dive deep into patient data [9]. For remote or telehealth patients, clinicians can securely send links for assessments, which automatically upload results to the patient’s EHR, ensuring smooth workflow continuity [2].
Jennifer Gozy, PsyD, LP, Director of Clinical Systems and Compliance at Care Counseling Clinics, explained:
"We are excited to expand our ability to track and report on data so that we can improve our quality assurance and reporting processes." [9]
This focus on integrated reporting also supports advanced longitudinal analysis for better patient care.
Ease of Longitudinal Analysis
Custom reporting tools within the platform help reveal patient trends over time, enabling clinicians to adjust treatments and identify issues early [8]. For example, visual trend tracking can highlight increasing anxiety levels before patients voice concerns [2]. This type of longitudinal insight is critical for value-based care, where reimbursements are tied to measurable outcomes [3]. Real-time dashboards further enhance care by identifying patterns that might indicate potential crises, allowing for timely intervention [2][10].
Opus Behavioral Health emphasizes that this level of data transparency helps organizations "identify trends, opportunities, and potential problems before they become critical and increase practice profits" [8]. Additionally, the platform is designed to align with and exceed Joint Commission (JCAHO) standards for patient feedback and measurement-based care [2].
Pros and Cons
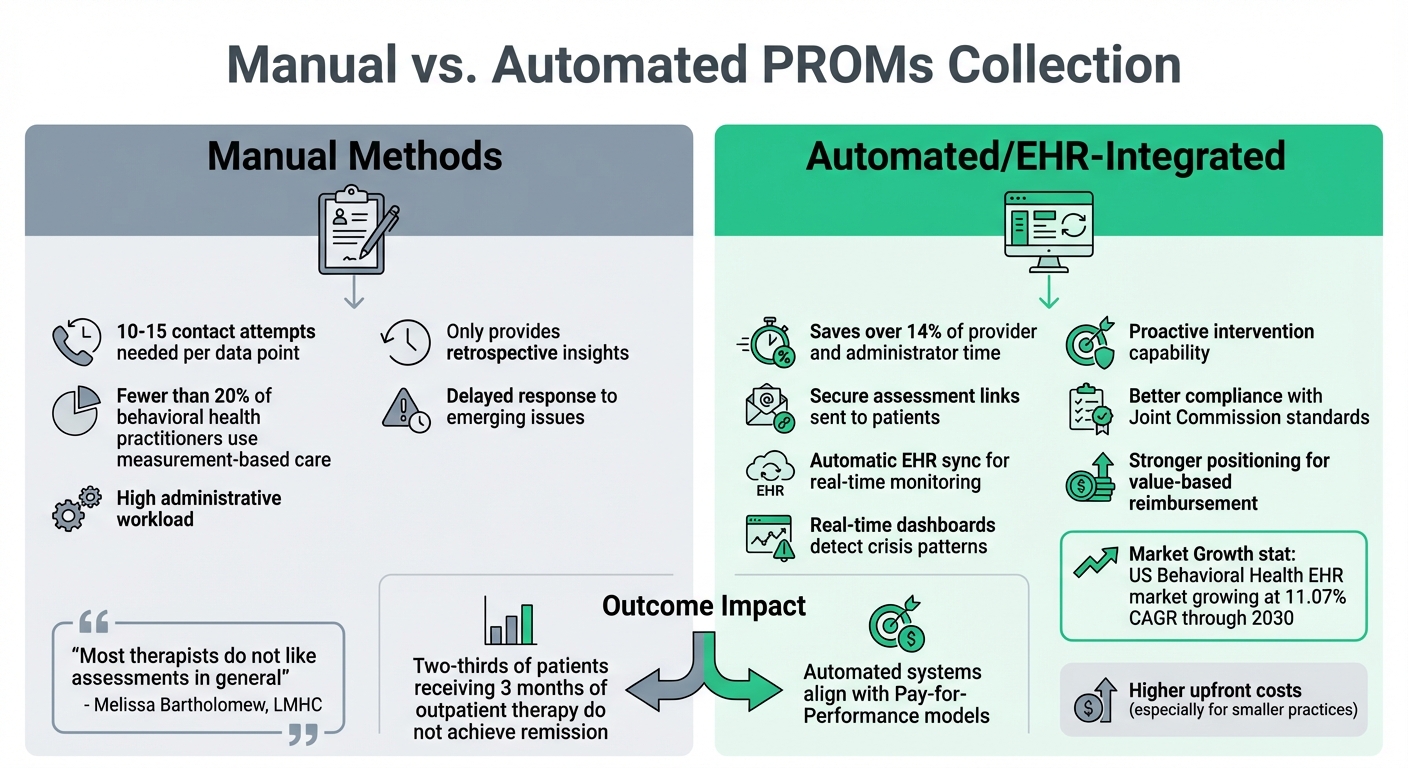
Manual vs Automated PROMs Collection in Behavioral Health Care
This section dives into the operational trade-offs between manual and automated approaches to tracking patient-reported outcome measures (PROMs) in behavioral health care, particularly in light of earlier discussions on integrated data collection.
When it comes to tracking patient outcomes, behavioral health providers face a choice: stick with manual PROMs collection or adopt automated, EHR-integrated systems. Both approaches have their own set of challenges and advantages, especially when considering operational demands and scalability. Manual methods, for example, come with a heavy workload. It takes 10–15 contact attempts to gather each data point manually [11]. For most clinicians, this level of effort is simply not feasible - especially since fewer than 20% of behavioral health practitioners currently use measurement-based care [14]. As Melissa Bartholomew, a Licensed Mental Health Counselor, pointed out:
"Most therapists do not like assessments in general" [14].
On the other hand, automation offers a way to simplify these time-consuming tasks.
Automated systems, like Opus Behavioral Health EHR, significantly reduce the workload by integrating tools that save over 14% of provider and administrator time [13]. Instead of relying on manual follow-ups and data entry, these systems send secure assessment links to patients and automatically sync the results back into the EHR for real-time monitoring [2]. This efficiency becomes even more relevant as the US Behavioral Health EHR market continues to grow at a compound annual growth rate (CAGR) of 11.07% through 2030 [12].
However, cost is a key factor. Automated tools can be expensive, which makes them less accessible for smaller practices [14]. Still, this upfront investment often brings long-term benefits, such as better compliance with Joint Commission standards and stronger positioning for value-based reimbursement contracts [2][3]. Another crucial advantage is how these systems address a gap in existing quality measures, which tend to focus on inpatient care - a setting that represents only a small fraction of behavioral health services [15].
Beyond cost considerations, the operational benefits of automation extend to crisis prevention. Manual systems only provide retrospective insights, which can delay responses to emerging issues. In contrast, automated systems with real-time dashboards can detect patterns that signal potential crises, allowing providers to act before situations escalate [2]. This proactive approach aligns well with the shift toward Pay-for-Performance models, especially given that two-thirds of patients receiving three months of outpatient therapy do not achieve remission [14].
Conclusion
When it comes to measurement-based care, the key is defining your mission and selecting metrics that drive meaningful results. A small outpatient clinic with just five clinicians will naturally prioritize differently than a 50-bed inpatient facility. For smaller practices, three financial metrics often stand out: clean claim rate (aim for over 90%), days in accounts receivable (keep it between 30–40 days), and denial rate (target under 5%) [16][17]. These metrics directly impact cash flow and long-term viability, creating a solid foundation for aligning clinical outcomes with value-based care initiatives.
For Pay-for-Performance models, start with validated clinical tools like the PHQ-9 and GAD-7 (Tier 1), as these meet reimbursement requirements. Once those are in place, expand to broader recovery markers (Tier 2) to improve patient outcomes [1][3]. Using integrated systems to track these measures in real time can streamline the process and improve care delivery.
It’s important to strike a balance between clinical relevance and operational efficiency. Experts emphasize that agreeing on a core set of measures can help reduce the administrative burden on providers [1]. Tools like Opus Behavioral Health EHR, which offers over 140 reporting options and real-time dashboards, can make this process more manageable.
Metrics should also align with the specific needs of your facility. Inpatient settings often benefit from tracking average length of stay and utilization efficiency, while outpatient centers may find greater value in monitoring 7-day and 30-day follow-up rates [3][1]. Regardless of the setting, keep in mind that fewer than 25% of nationally endorsed quality measures are patient-reported outcomes [1]. Adding tools like patient experience surveys or the Net Promoter Score can help address these gaps [3].
Ultimately, focus on metrics that align with your reimbursement model and patient priorities. Invest in automation tools that integrate smoothly into your team’s workflow. The best metrics are those that your staff can consistently track and act upon.
FAQs
How do tools like PHQ-9 and GAD-7 help improve patient outcomes in behavioral health?
Tools like the PHQ-9 (Patient Health Questionnaire-9) and GAD-7 (Generalized Anxiety Disorder-7) are essential for gathering self-reported data on mental health symptoms. This information gives clinicians a clearer picture of a patient’s condition and helps track changes over time.
Incorporating these Patient-Reported Outcome Measures (PROMs) into care plans allows providers to customize treatments based on individual needs, pinpoint areas that may need adjustments, and create a more patient-focused approach. These tools also support continuous monitoring, helping ensure that treatments remain effective and aligned with the patient’s recovery goals.
What are the advantages of using EHR systems for real-time data collection in behavioral health care?
Integrating Electronic Health Record (EHR) systems for real-time data collection in behavioral health care brings a host of benefits. It enhances communication among providers, simplifies care coordination, and enables up-to-the-minute tracking of patient outcomes. These systems also play a critical role in supporting value-based care by facilitating accurate reporting and measurement-based treatment approaches, ensuring patients receive care tailored to their needs.
With real-time data at their fingertips, providers can make quicker, well-informed decisions, boosting both the quality and efficiency of care. The result? Better patient outcomes, higher satisfaction levels, and smoother operations for behavioral health organizations.
Why is it important to prioritize outcome metrics over process metrics in behavioral health reporting?
When it comes to behavioral health reporting, outcome metrics take center stage. These metrics measure the real-world impact of care on a patient's progress and overall well-being. Unlike process metrics - which focus on tracking administrative or procedural steps - outcome metrics zero in on the effectiveness of treatments and how satisfied patients are with their care.
By prioritizing outcomes, providers can pinpoint what’s truly effective, make informed improvements, and align their practices with value-based care models that prioritize quality over sheer volume. This shift not only improves the level of care patients receive but also ensures providers meet industry standards and reporting requirements.
