Choosing Electronic Billing Software for Behavioral Health Practices Wisely
Behavioral health practices require billing software that effectively handles complex coding, regulatory compliance, and revenue cycle management.
Key considerations include:
Regulatory Compliance: Software must support HIPAA, ICD-10, CPT, and, where applicable, 42 CFR Part 2 for substance use disorder records.
Integration: Look for systems that unify EHR, CRM, and billing to reduce errors and improve efficiency.
Automation: Features like automated claims processing, insurance verification, and appointment reminders can save time and reduce denial rates.
Cost: Pricing varies widely, with options for solo practitioners starting around $50/month and enterprise solutions exceeding $150/month.
Top Options:
Opus Behavioral Health EHR: Offers robust compliance, AI-powered documentation, and full integration across EHR, CRM, and billing.
TheraBill: Strong focus on compliance and automation but works best with WebPT EMR.
SimplePractice: Combines billing, scheduling, and documentation but may lack advanced features for larger practices.Quick Comparison:
|
Feature |
Opus Behavioral Health EHR |
TheraBill |
SimplePractice |
|---|---|---|---|
|
Compliance |
HIPAA, 42 CFR Part 2 |
HIPAA, BAA included |
HIPAA, BAA included |
|
Integration |
Unified EHR/CRM/RCM |
Best with WebPT EMR |
All-in-one EHR |
|
Automation |
AI-powered, text-to-pay |
Claim scrubbing, ERA |
AutoPay, ERA, EFT |
|
Cost |
Custom pricing |
$149/month/provider |
$49–$99/month |
|
Best For |
Mid to large practices |
WebPT users |
Solo/small practices |
Evaluate your practice’s size, denial rates, and specific needs to choose the right software. A well-suited platform can simplify billing, improve compliance, and support better financial outcomes.
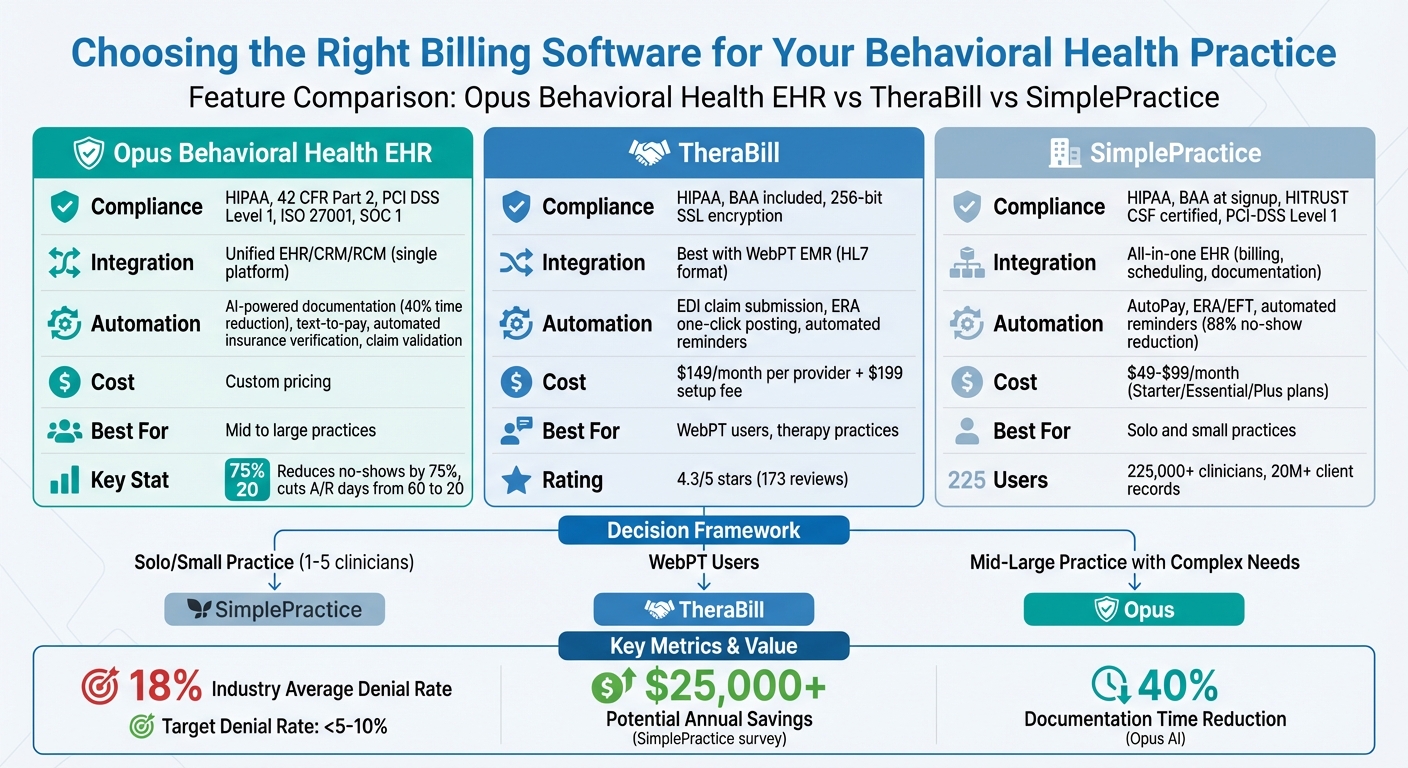
Behavioral Health Billing Software Comparison: Opus vs TheraBill vs SimplePractice
1. Opus Behavioral Health EHR
Regulatory Compliance
Opus Behavioral Health EHR is tailored to meet the specific compliance requirements of behavioral health practices. It adheres to stringent regulatory standards, ensuring the protection of sensitive patient information.
The platform complies with HIPAA Privacy, Security, and Breach Notification Rules, a critical safeguard for addiction, SUD, and mental health treatment centers managing protected health information (PHI).
Additionally, Opus holds certifications like PCI DSS Level 1 for secure payment processing, ISO 27001 for global information security, and SOC 1/SSAE 16/ISAE 3402 for financial reporting and internal controls [3].
"Protecting Your Data is our Highest Priority with Security and Compliance." – Opus Behavioral Health [3]
To bolster security further, Opus employs multi-factor authentication (MFA), single sign-on (SSO), and 24/7 intrusion monitoring enhanced by threat intelligence.
Communications are safeguarded through Transport Layer Security (TLS) with 2048-bit encryption, and user session tokens are secured with 256-bit encryption (JWT with HMAC-SHA256) [3].
Practices can also set access restrictions based on location, IP addresses, and time of day to protect billing and clinical data. These security measures integrate seamlessly into Opus's unified system.
EHR Integration
Opus combines CRM, EHR, and RCM into a single platform, eliminating the need for manual data entry and ensuring that clinical documentation flows effortlessly into billing workflows.
Through its partnership with Dazos, the platform enables a bidirectional exchange of information between EHR and CRM systems via single sign-on.
David Farache, Co-founder and CEO of Dazos, highlighted this synergy: "The single sign-on feature for the integrated EHR/CRM platform and the resulting bidirectional flow of information between these two great systems is an industry game changer" [6].
The integrated lab module simplifies operations by allowing clinicians to order tests and receive results directly within the EHR. Additionally, the e-prescribing feature draws from clinical notes, diagnoses, and patient history to minimize errors.
With over 160,000 practitioners using the platform daily, Opus has proven its ability to handle high-volume operations efficiently [4]. This integration sets the stage for further automation to streamline administrative processes.
Automation Features
Opus incorporates Copilot AI, an integrated scribe tool that drafts progress notes for both telehealth and in-person sessions, reducing documentation time by 40% [4].
This tool ensures that every billable session is paired with accurate clinical notes. Beyond documentation, Opus automates essential administrative tasks like insurance verification, lead routing, and task management, covering processes from booking to billing and handling both UB-04 and CMS 1500 claims[4].
"By leveraging automated data processing, it minimizes errors in group sessions." – Judd Carey, Director of Operations, Mindful Health [4]
The platform also integrates with services like Curogram to support Text-to-Pay workflows, allowing secure payment links to be sent to guarantors and syncing payment data back to the EHR [5].
Amanda Wilson, Director of Clinical Services at a Mental Health and Substance Use Treatment Center, noted, "This process will simplify our operations to save so much time.
We will no longer have to manually pull so many charts per quarter and have a timelier billing process for quicker reimbursements" [4].
Automated appointment reminders further enhance efficiency, reducing no-shows by up to 75%, while text-to-pay features cut accounts receivable days from 60 to 20 [5].
Cost-Effectiveness
Opus offers access to over 140 practice management reports, enabling practices to monitor financial performance and pinpoint revenue cycle bottlenecks [4].
Trevor Mulvey, VP of Finance at Care Counseling Clinics, explained their choice: "We chose OPUS for... robust functionality for our back-office support, payor rate compliance features, and accrual accounting reporting" [4]. By automating billing workflows and minimizing manual data entry, staff can dedicate more time to patient care.
The platform's automated insurance verification and real-time claim validation help reduce the industry-average claim denial rate of roughly 18% [2].
With 24/7 customer support, billing teams can quickly resolve issues, minimizing revenue disruptions. These efficiencies not only improve revenue cycle management but also enhance the overall quality of patient care.
2. TheraBill
TheraBill stands out as a noteworthy option for electronic billing, offering a focus on strong compliance measures and efficient automation.
Regulatory Compliance
TheraBill prioritizes HIPAA compliance by employing 256-bit SSL encryption and enforcing strict password protocols. It ensures the secure handling of Protected Health Information (PHI) through Business Associate Agreements (BAA).
The platform also includes nightly cloud-based data backups and provides secure provider portals for managing sensitive information.
To further reduce errors, TheraBill incorporates multiple layers of claim scrubbing, flagging inaccuracies and returning claims for correction within two days. This thorough process helps ensure accurate coding and reduces the risk of compliance issues.
EHR Integration
As part of the WebPT family, TheraBill integrates seamlessly with the WebPT EMR system. This connection allows patient demographics, payments, and clinical notes to transfer smoothly via the HL7 file format.
For example, daily notes entered in WebPT are automatically converted into billing sessions, streamlining insurance invoicing.
However, some users have noted challenges when using TheraBill with third-party EHR systems. Tameka from Medical Practice shared her experience:
"The separation from my EMR makes things tricky. If a patient’s insurance details are entered incorrectly into the WebPT EMR and then transferred to Therabill, it gets stuck with the wrong provider" [10].
Despite these occasional integration hurdles, the connection with WebPT enhances TheraBill’s automation capabilities, simplifying billing workflows.
Automation Features
TheraBill automates the submission of HIPAA-compliant EDI claims to a vast network of insurance companies and government payers, eliminating the need for individual clearinghouse accounts [7][8].
Its Electronic Remittance Advice (ERA) feature allows one-click posting of insurance and patient payments, automatically attributing payments to the correct accounts.
Muhammad from Hospital & Health Care highlighted its ease of use:
"The system is really easy to use as it is fast and responsive, and it populates all the necessary information with just a single click" [9].
Additionally, the platform includes automated reminders to help reduce no-shows and lighten the workload for front-office staff [8][9].
Cost-Effectiveness
TheraBill offers a straightforward pricing structure: $149 per provider per month, with a one-time $199 setup fee. Unlike some competitors, it does not charge per-claim or clearinghouse fees.
Subscribers benefit from unlimited staff logins, 2 GB of attachment storage, and email support [9][11]. User feedback suggests that 70% of reviewers appreciate its billing and claims management features [9].
The software has earned a 4.3/5-star rating from 173 reviews on SoftwareReview.com [12].
Obaid from Amro Healthcare praised the platform, saying:
"Therabill is a reliable and user-friendly software for therapy practices, making scheduling, documentation, and billing seamless" [9].
3. SimplePractice
SimplePractice is a comprehensive platform that combines billing, scheduling, and clinical documentation into one system. With over 225,000 private practice clinicians nationwide using it [13], it’s become a go-to tool for streamlining administrative tasks.
Regulatory Compliance
From the moment an account is created - whether it’s a trial or paid subscription - SimplePractice ensures immediate HIPAA compliance by providing a signed Business Associate Agreement (BAA) [13].
It also holds HITRUST CSF certification and uses bank-level security measures with 24/7 server monitoring [20,21]. Jill Shook MS, CCC-SLP, emphasizes this feature:
"SimplePractice secures client data with a signed BAA at account creation." [13]
For payment processing, SimplePractice partners with Stripe, which is PCI-DSS Level 1 compliant, offering the highest industry standard for payment security [21,22].
The platform also integrates essential coding tools, like DSM, ICD-10, and CPT codes, which automatically populate into treatment plans and claims, ensuring accuracy and compliance [14]. These built-in protections and tools make it easier to maintain regulatory standards without added effort.
EHR Integration
SimplePractice streamlines operations by integrating billing, scheduling, progress notes, treatment plans, and client portal features into one cohesive system [14].
This eliminates the hassle of transferring data between systems or juggling multiple apps [16]. The platform automatically generates invoices, superbills, and CMS-1500 claims directly from appointments, cutting down on manual data entry [19,21].
However, practices with multiple clinicians may encounter some limitations, such as siloed records. Additionally, the platform doesn’t currently support UB-04 facility claims, which are required for certain institutional behavioral health billing needs [19].
Automation Features
SimplePractice’s automation tools are designed to save time and reduce manual work. Features like AutoPay allow client payments to be processed automatically using stored cards [15].
Insurance payments are streamlined with Electronic Remittance Advice (ERA) and Electronic Funds Transfer (EFT), enabling direct deposits into business accounts [19,20]. Automated appointment reminders - sent via text, phone, or email - help practitioners reduce no-shows by 88% [17].
The platform also simplifies clinical coding by automatically transferring information from documentation into billing forms.
A 2025 survey of 906 practitioners reported that using SimplePractice’s documentation tools saved practices over $25,000 annually in administrative costs [17].
Cost-Effectiveness
SimplePractice offers three pricing tiers to fit different needs:
Starter Plan ($49/month): Includes core EHR features and electronic claim filing.
Essential Plan ($79/month): Adds appointment reminders and calendar syncing.
Plus Plan ($99/month): Includes group telehealth and automatic insurance status checks, with additional clinicians costing $74 each [20].New users can take advantage of a 30-day free trial without needing a credit card, along with free credentialing services [20,24].
As of October 2025, SimplePractice has earned top ratings on third-party platforms, a 96% satisfaction rate among practitioners [18], and manages records for over 20 million clients [17]. These features make it a strong contender for practices looking to streamline their operations.
Advantages and Disadvantages
Let’s explore the strengths and possible challenges of using Opus Behavioral Health EHR in your practice, building on the features discussed earlier.
One of the standout benefits is its native integration across EHR, CRM, and RCM systems. This eliminates the gaps in data mapping that can lead to missing charges or delayed claims [1].
For example, automated workflows ensure that scheduling is blocked when authorization limits are reached, preventing the 2–3 week delays caused by errors only discovered after claim submission [2].
Additionally, the platform’s AI-powered documentation and detailed reporting provide complete oversight, while real-time claim validation helps address the 18% in-network denial rate that’s common in the industry [2].
By unifying these processes, Opus simplifies billing, reduces manual errors, and lightens the administrative workload. Its design not only streamlines revenue cycles but also ensures compliance with the regulatory standards that are so important in behavioral health practices.
This unified approach demonstrates Opus’s focus on efficiency and accuracy, key factors for any behavioral health provider. Up next, we’ll summarize these insights to help you make an informed decision about whether this software is the right fit for your needs.
Conclusion
When choosing electronic billing software, it’s essential to consider how well it aligns with your practice’s specific needs.
Factors like practice size, revenue model, and clinical focus play a big role in finding the right fit. For solo clinicians or small practices, systems priced between $50 and $150 per month often work best, especially if they focus on ease of use and quick setup.
Mid-sized practices, particularly those managing specialized programs like ABA therapy or substance use disorder treatment, may require systems with advanced features like revenue cycle management and authorization tracking.
On the other hand, larger organizations with multiple locations typically benefit from enterprise-grade platforms that offer advanced analytics and multi-site functionality.
Before making a decision, it’s a good idea to calculate your denial rate (percentage of rejected claims). If the denial rate exceeds 5–10%, it could indicate significant revenue loss and inefficiencies in your current system.
This metric can guide your evaluation process. During software demonstrations, pay close attention to how the system manages authorization limits. The best platforms will automatically block scheduling once a patient's approved hours are used up, helping to avoid unnecessary revenue delays.
Involve your billing team in the evaluation process and ensure the vendor provides a signed Business Associate Agreement (BAA) that includes export rights for clinical records. Confirm that the software supports HIPAA compliance and, if applicable, adheres to 42 CFR Part 2 regulations for substance use disorder programs.
Modern practices increasingly benefit from unified platforms that combine CRM, EHR, and revenue cycle management into a single system. These platforms help eliminate data silos and reduce manual errors, which are common causes of claim denials. As Shameem C Hameed, Founder of blueBriX, aptly puts it:
"Behavioral health is no longer on the healthcare fringe - it's front and center." [21]
Ultimately, choose software that meets today’s regulatory demands while scaling with your practice’s growth. A well-chosen platform can streamline operations, improve compliance, and support your team in delivering quality care.
FAQs
How do I know if my billing software supports 42 CFR Part 2?
If you’re wondering whether your billing software complies with 42 CFR Part 2, here’s what to look for. Check if it includes essential features like SUD (Substance Use Disorder) record segmentation, access controls, and consent tracking. These tools are key to managing patient consent for disclosures and keeping records properly segmented when required.
If you’re not sure about your software’s capabilities, reach out to your provider. They can confirm whether these compliance features are built into the system. It’s always better to double-check than to risk non-compliance.
What billing automations reduce denials the most?
Billing automation tools can play a big role in cutting down claim denials. Features like integrated authorization, session-to-billing code automation, real-time claims tracking, error detection, and auto-generation of appeals work together to tackle issues before they become problems. By catching errors early, these tools help reduce the common reasons for claim rejections, making the entire billing process smoother and more efficient.
What should I ask in a billing software demo?
When you're checking out a billing software demo, it's important to dig into the features that matter most for your practice. Here are some key questions to ask:
Billing workflows: How does the software manage tasks like insurance claims and payment processing?
Automation: What tools are included to minimize manual errors and save time?
Compliance and security: Is the software designed to meet behavioral health regulations and ensure data security?
Integration capabilities: Can it seamlessly connect with your EHR system?
Training and support: What kind of onboarding, training, and ongoing support does the provider offer?These questions will help you figure out if the software aligns with your practice's specific needs.
