AI in Behavioral Health: Retention Challenges Solved
Behavioral health centers face a big challenge: keeping patients engaged in their care.
Missed appointments can disrupt recovery, lead to relapse, and cost treatment centers thousands of dollars annually. Traditional outreach methods like phone calls and patient portals often fall short.
AI-powered tools are changing the game. Automated SMS reminders, real-time data tracking, and two-way texting are helping reduce no-show rates by up to 30%.
These tools simplify communication, lighten staff workloads, and improve patient engagement. For example, a Texas outpatient center using AI dropped their no-show rate from 22% to 10%, recovering $78,000 in annual revenue.
Key takeaways:
Missed appointments hurt recovery and cost centers over $100,000 annually.
AI tools like SMS reminders and predictive analytics reduce no-shows and identify at-risk patients.
Automation saves staff time, reduces burnout, and ensures consistent communication.AI isn't just about saving time - it’s about helping patients stay on track during vulnerable moments. Solutions like Opus Behavioral Health EHR combine automated communication, real-time insights, and advanced reporting to tackle retention challenges effectively.
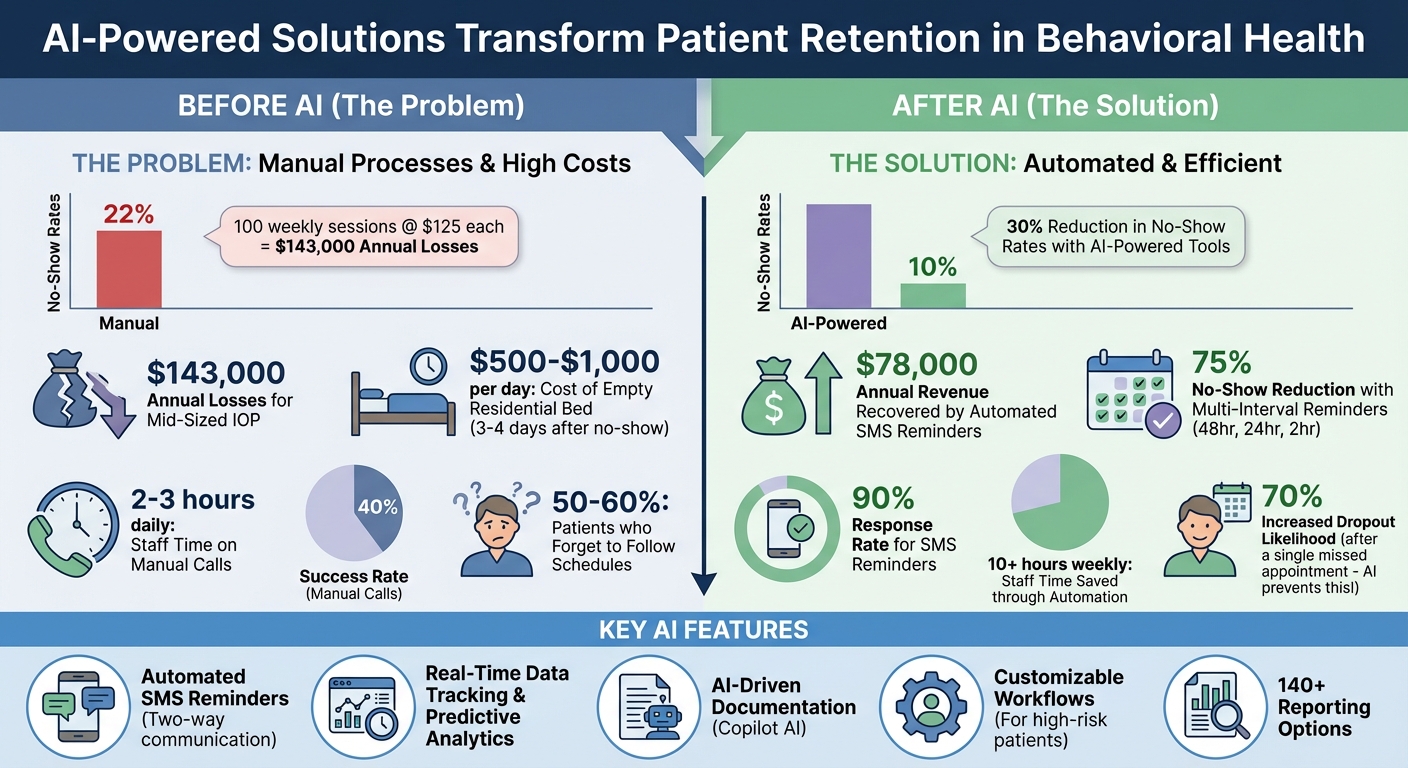
AI Impact on Behavioral Health Patient Retention: Key Statistics and Cost Savings
Patient Retention Challenges in Behavioral Health
Retention in behavioral health care is a complex issue, often influenced by a mix of factors. Both patients and providers face hurdles that can disrupt consistent care. These challenges are multifaceted, but AI-powered tools are increasingly seen as a way to address them.
Motivation and Engagement Barriers
For patients in early recovery or those managing severe mental health conditions, tasks like scheduling and attending appointments can feel overwhelming.
This is often due to "brain fog", a common symptom that affects memory, planning, and the ability to follow through on commitments [1]. Even seemingly simple responsibilities can feel insurmountable [3].
Adding to this is the cycle of shame. Missing a therapy session can leave patients feeling embarrassed or judged, which often discourages them from returning to treatment.
As Curogram explains:
"Shame is a powerful force in recovery. Patients who miss a session often feel embarrassed... This shame can stop them from coming back." – Curogram [3]
When appointments are missed, it can disrupt the recovery process and lead to feelings of isolation - one of the leading factors contributing to relapse [3].
Operational and Logistical Challenges
From the provider's perspective, administrative inefficiencies make patient retention even more difficult. Staff often spend hours manually confirming appointments, yet only achieve a 40% success rate due to unanswered calls and missed voicemails [2].
High clinician burnout further complicates matters. Excessive documentation and administrative tasks contribute to therapist turnover, which forces patients to start over with new providers. This disruption can weaken trust and derail progress.
As U.S. Surgeon General Vivek Murthy has pointed out:
"The nation's health depends on the well-being of our health workforce... Confronting the long-standing drivers of burnout among our health workers must be a top national priority." – Vivek Murthy, U.S. Surgeon General [5]
These inefficiencies highlight how AI-driven automation could ease administrative burdens and improve both patient and provider experiences.
Impact of Life Stressors
External stressors like financial struggles, work obligations, and family responsibilities add another layer of difficulty. For many patients, balancing these demands while managing behavioral health conditions can make attending therapy feel unmanageable. In fact, 50% to 60% of patients report forgetting to follow their recommended schedules [6]. This underscores the challenge of maintaining consistent care while navigating the complexities of daily life and mental health struggles.
How Retention Challenges Affect Treatment Centers
When patient retention issues arise, treatment centers face a ripple effect that impacts their ability to deliver care and maintain financial stability.
Retention problems go beyond empty appointment slots. They bring clinical, financial, and operational obstacles that can jeopardize the quality of care and the center's overall sustainability.
Disruption to Patient Progress and Outcomes
Every missed session isn’t just a gap in the schedule - it’s a break in a patient’s recovery journey.
As Mira Gwehn Revilla puts it:
"A missed visit at your treatment center is not just a gap in the day. It is a break in clinical care that can put a patient's recovery at risk." – Mira Gwehn Revilla, Author [1]
Recovery thrives on consistency. Regular sessions help patients build momentum, while missed appointments can derail progress [3].
These gaps make it harder for clinicians to detect early warning signs like heightened stress or emerging triggers [3]. This becomes especially critical during transitional phases, such as moving from detox to outpatient care. Without consistent engagement, weeks of progress can be undone [3].
Operational disruptions caused by retention challenges also lead to financial losses and difficulties in managing patient data.
Financial Strain on Providers
Retention issues directly affect a facility's bottom line. For example, a mid-sized Intensive Outpatient Program (IOP) facility in Texas reported a 22% no-show rate in February 2026 while relying on manual processes. With 100 weekly sessions priced at $125 each, the facility was losing $2,750 every week - adding up to $143,000 annually [2].
For residential programs, the financial impact is even more pronounced. A single no-show on intake day can leave a bed empty for 3–4 days, costing between $500 and $1,000 per day [2].
On top of that, staff spend 2–3 hours daily making manual reminder calls, often achieving only a 40% confirmation rate [2]. These administrative demands pull resources away from patient care.
Insurance requirements add another layer of complexity. Many payers mandate proof of patient engagement for continued stay authorizations. Low attendance rates can result in denied claims and lost revenue opportunities down the road [2].
Challenges to Research and Data Accuracy
Retention issues also compromise the accuracy of clinical records. Missed sessions and early discharges often leave behind incomplete documentation - missing signatures, blank form fields, and fragmented treatment histories that can’t be retroactively fixed [7].
As Mira Gwehn Revilla explains:
"Charts become riddled with gaps. Auditors find missing signatures weeks later. This is where clinical data integrity starts to break down. Not from bad intent, but from bad process." – Mira Gwehn Revilla, Curogram [7]
These documentation gaps can cause significant problems during audits by CARF, the Joint Commission, or state agencies, where surveyors expect fully completed records with proper timestamps and signatures [7].
Beyond compliance, incomplete records hinder efforts to track long-term outcomes or measure the effectiveness of treatments [3].
They also limit the potential of AI-driven tools, which rely on clean, comprehensive data to identify retention risks and improve care delivery. This highlights the importance of adopting solutions like Opus Behavioral Health EHR to address these systemic challenges effectively.
AI-Powered Insights for Identifying Retention Risks
AI is reshaping how retention risks are managed by using real-time data to spot potential problems before they escalate. By identifying at-risk patients early, treatment centers can implement tailored interventions to address these challenges effectively.
Predicting Dropout Risks with Data Analytics
AI systems work seamlessly with Electronic Health Records (EHR) to track patient behavior in real time. For example, a single missed appointment isn't just a minor scheduling issue - it increases the likelihood of patient dropout by 70% [8].
By analyzing patterns like frequent cancellations, unresponsiveness to prompts, or repeated no-shows, AI flags potential risks early [3].
The technology goes beyond attendance data. It can identify patients facing challenges like "cognitive fog", which is common in early recovery [1].
For those struggling with tasks such as logging into portals or managing complex schedules, AI suggests simpler communication methods like SMS [1]. Additionally, by analyzing therapy session details, the system evaluates which treatments are most effective, helping predict whether a patient is likely to make progress or fall behind [4].
Risk stratification plays a crucial role in tailoring care. For instance, patients in their first week post-detox - when dropout rates are highest - might receive more frequent check-ins, while stable outpatient clients stick to standard reminders [1].
As Mira Gwehn Revilla from Curogram explains:
"Disengagement is a warning sign. It signals that something has changed... the missed session is a red flag" [3].
Personalized Engagement Through AI
Once high-risk patients are identified, AI steps in with personalized re-engagement strategies. For example, two-way SMS systems simplify communication - patients can confirm appointments by simply replying "C" [1][3]. This method is highly effective, with SMS achieving a 90% response rate compared to around 40% for traditional phone calls [2].
AI also customizes reminder messages based on the patient's care plan. For example, patients on Medication-Assisted Treatment (MAT) receive medication-specific instructions, while those in detox are reminded of exact check-in times [3].
For high-risk patients, reminders are sent at intervals of 48, 24, and 2 hours before appointments - a schedule shown to reduce no-shows by up to 75% [1]. If a cancellation does happen, the system immediately notifies case managers, enabling them to initiate safety checks or clinical outreach to maintain continuity of care [3].
Tracking Outcomes for Continuous Improvement
AI doesn’t stop at identifying risks and personalizing engagement - it also tracks outcomes to refine treatment approaches.
By collecting and analyzing structured data on patient progress, these tools help clinicians determine which interventions are most effective for different types of patients [4]. AI also examines session trends to provide actionable insights, guiding therapists toward strategies that yield better results [4].
This ongoing tracking has dual benefits. It allows clinicians to make real-time adjustments to treatment plans and creates a solid data record for long-term improvements. Automated documentation provides clear, searchable audit trails, which are invaluable during insurance audits or authorization renewals.
This supports the operational goals discussed earlier by demonstrating a facility’s commitment to patient retention [1]. Over time, clean and comprehensive data strengthens predictive models, helping refine care strategies and improve overall retention rates.
AI Automation Solutions for Better Retention
AI-powered insights are great for spotting at-risk patients, but automation takes things further by cutting down the administrative workload that often stops staff from acting on those insights. By automating communication and simplifying workflows, treatment centers can stay in touch with patients consistently without overloading their teams. This blend of automation and data-driven insights helps improve both operations and patient engagement.
Streamlining Administrative Workflows
In many behavioral health facilities, manual appointment reminders eat up 2–3 hours of staff time each day [2]. AI-powered systems eliminate this time drain by syncing directly with EHR schedules in real time. They automatically send SMS alerts tailored to the type of visit - whether it’s a detox check-in, therapy session, or group counseling [1].
The results speak for themselves. Facilities using automated reminders can save 10 or more hours of staff time every week [2]. This allows staff to focus more on patient care rather than repetitive admin tasks, which also helps reduce burnout - a key factor in maintaining quality care. Plus, two-way SMS communication makes life easier for patients, too. For instance, they can confirm appointments with a single letter, like "C", which is especially helpful for those in early recovery dealing with executive function challenges [1].
Automation also steps in when cancellations happen. The system instantly notifies the front desk, enabling staff to message waitlisted patients and fill open slots within minutes [2].
This not only prevents revenue loss but also keeps schedules running smoothly. On top of that, tools like Opus Copilot AI can turn spoken session notes into organized, insurance-ready clinical documentation. This saves clinicians time, ensures documentation is audit-ready, and makes records easy to search [1].
These workflow upgrades naturally tie into stronger patient communication through unified telehealth and CRM platforms.
Improving Communication with CRM and Telehealth
With streamlined workflows in place, AI-driven communication systems take patient engagement to the next level. AI-powered CRMs solve a common issue: patients who "fall through the cracks" during intake or care transitions.
These systems track patients throughout their care journey, using automated lead routing and timely follow-ups to keep everything on track [9]. Rebeka Tolle, VP of Operations at Care Counseling Clinics, highlights this benefit:
"We are looking forward to the ease with which clients can schedule their appointments and receive communications for their ongoing care all in one place" [9].
Unified telehealth platforms combine video conferencing, scheduling, and documentation into one seamless experience. This makes it easier for patients to navigate their care, especially those dealing with "brain fog" during early recovery [1].
Features like text-to-pay let patients handle co-pays or balances before arriving, reducing the hassle of check-in and improving collection rates [2].
These CRM and telehealth tools also expand on the benefits of two-way SMS communication. By maintaining regular contact between sessions, they help fight isolation - a major relapse risk - while reinforcing that patients are valued and supported by their care team [3].
Opus Behavioral Health EHR: AI Tools for Patient Retention
Opus Behavioral Health EHR tackles patient retention challenges head-on with AI-driven solutions. By combining automated communication, intelligent documentation, and detailed reporting, the platform helps treatment centers keep patients engaged throughout their recovery while reducing administrative workloads. These tools empower clinicians to identify and address disengagement early, preventing dropouts and supporting long-term recovery. Let’s dive into how these AI-powered features address specific retention obstacles.
AI-Driven Documentation and Outcomes Measurement
With Copilot AI, spoken session notes are instantly converted into structured, audit-ready records. This eliminates the need for manual note-taking, saving clinicians hours of work while ensuring compliance with searchable documentation [1].
The platform also includes tools to measure patient outcomes across multiple areas, offering a detailed view of how individuals respond to treatment. Paired with automated SMS reminders, this feature creates an early warning system for disengagement. As Mira Gwehn Revilla explains, "A missed visit is often the first warning sign of a relapse. When a patient stops showing up, it may mean they are struggling" [1]. Every automated outreach attempt and patient response is logged, creating a complete audit trail for insurance reviews and accreditation.
One success story comes from a Texas-based outpatient facility that transitioned from manual calls to Opus EHR’s automated SMS reminders. Their no-show rate dropped from 22% to 10%, saving about 12 sessions per week and recovering nearly $78,000 in annual revenue [2]. This example highlights how AI-powered communication can directly impact patient retention and financial outcomes.
Customizable Workflows and Advanced Reporting
Opus Behavioral Health EHR offers over 140 reporting options, giving treatment centers the ability to analyze retention trends and evaluate engagement strategies. These reports pull data from appointment histories, communication logs, and clinical outcomes, providing a full picture of patient engagement.
The system also features customizable workflows, allowing facilities to tailor reminder schedules and communication patterns based on patient needs. For example, high-risk patients recently discharged from detox can receive reminders at 48 hours, 24 hours, and the morning of their appointment to combat cognitive challenges [1]. If a patient cancels or doesn’t confirm an appointment, the system flags this for case managers, enabling them to quickly intervene. Open slots can then be offered to waitlisted patients, ensuring no time is wasted [2][3].
These tools not only improve daily operations but also adapt to the unique requirements of each practice, whether small or large.
Scalability for Practices of All Sizes
Opus Behavioral Health EHR offers three subscription tiers to accommodate practices of varying sizes:
Basic Plan: Designed for small practices (1–10 clinicians), it includes essential EHR, CRM, basic RCM, telehealth, and customizable workflows.
Standard Plan: Geared toward mid-sized practices (11–20 clinicians), adding advanced RCM, AI-powered documentation, and lab integration.
Premium Plan: Built for larger practices (21+ clinicians), offering enhanced reporting and comprehensive outcomes measurement tools.This tiered system allows even small clinics to start with core features like automated reminders and basic engagement tracking.
As they grow, they can seamlessly scale up to include predictive analytics and more advanced tools. All plans come with two-way SMS integration and automated workflows, ensuring streamlined communication and reduced administrative tasks for practices of any size [2].
Conclusion
Patient retention in behavioral health isn’t just about keeping schedules full - it’s about protecting patients during their most vulnerable times. AI-powered tools are stepping in to tackle key challenges like cognitive barriers, communication breakdowns, and the administrative burdens that pull staff away from patient care.
For example, facilities using automated SMS reminders have seen no-show rates drop from 22% to 10% [2]. These tools act as an early warning system, identifying disengagement before it escalates into relapse.
As Mira Gwehn Revilla aptly puts it:
"Clinical adherence in behavioral health is not just about filling time slots. It is about keeping patients safe during their most fragile moments" [3].
These results don’t just benefit patients - they also streamline clinical workflows. With features like AI-driven documentation, two-way texting that boasts a 90% response rate, customizable workflows, and advanced reporting, Opus Behavioral Health EHR helps reduce paperwork and identify at-risk patients [2].
By combining automation with data analytics, treatment centers can improve retention and build a more sustainable care model.
The choice for behavioral health centers is clear: stick with outdated manual processes or embrace AI-driven solutions that free up staff time, secure revenue, and maintain patient engagement. With today’s technology, retention is no longer an uphill battle - it’s a manageable, data-informed process that strengthens both care outcomes and operational efficiency.
FAQs
How does AI predict which patients are likely to drop out?
AI can predict which patients are at risk of dropping out by analyzing patterns in ePRO (electronic patient-reported outcomes) usage, wearable device data, and other diverse inputs. By identifying these patterns, it can forecast dropout risks hours or even days ahead. This allows for timely and targeted interventions, helping to keep patients engaged and improve overall retention rates.
How do two-way SMS reminders improve appointment attendance?
Two-way SMS reminders make it simple for patients to confirm, cancel, or reschedule appointments with just a quick reply. This kind of direct communication helps keep patients on track with their treatment plans, reduces missed appointments, and ensures care stays consistent.
What should a behavioral health center consider before using AI automation?
Before bringing AI automation into the mix, behavioral health centers need to carefully assess how it fits within their current workflows and tools, such as Opus Behavioral Health EHR. This step is crucial to improving efficiency without disrupting daily operations.
Key considerations include:
HIPAA compliance: Ensuring any AI tools meet strict privacy and security standards to protect sensitive patient information.
Accuracy of AI features: Evaluating how reliable AI-driven tools are, such as automated appointment reminders, to avoid errors that could impact patient care.
Staff training: Equipping team members with the knowledge to understand and use AI-generated insights effectively.It's also essential to think about how AI can help reduce administrative tasks while still preserving the personalized care and oversight that patients depend on. Balancing these factors ensures that automation becomes a helpful asset rather than a hindrance.
