Behavioral Health Practice Billing Software That Boosts Revenue
Behavioral health practices often struggle with billing complexities like high denial rates, coding errors, and insurance challenges.
Specialized billing software can help solve these issues, improve claim acceptance, and increase revenue.
Here’s a quick look at three top platforms:
Opus Behavioral Health EHR: Ideal for mid-sized practices, it offers automated tools like insurance verification, AI-powered documentation, and text-to-pay. It reduces no-show rates and speeds up payments to as few as 20 days.
TheraBill: Best for smaller practices, it provides unlimited claim submissions, error-checking, and automated reminders. Pricing starts at $149/month per provider.
SimplePractice: Designed for solo and small groups, it combines billing, scheduling, and telehealth. Plans range from $29–$99/month, with features like automated no-show fees and credentialing support.Each platform addresses billing challenges differently, making it easier for practices to manage claims, reduce denials, and improve cash flow. Below is a quick comparison of their features.
Quick Comparison
|
Feature |
Opus Behavioral Health EHR |
TheraBill |
SimplePractice |
|---|---|---|---|
|
Target Practice Size |
Mid-sized to large |
Small to medium |
Solo to small groups |
|
Key Features |
AI-driven notes, text-to-pay, 140+ reports |
Unlimited claims, ERA, appointment reminders |
Telehealth, no-show fees, credentialing |
|
Starting Price |
Custom pricing |
$149/month per provider |
$29/month |
|
Claim Submission |
Automated with error checks |
Unlimited electronic claims |
10–35 claims/month included |
|
Payment Processing |
Text-to-pay |
Integrated credit cards |
Stripe integration |
|
No-Show Rate Reduction |
Yes (via SMS reminders) |
Yes (via email/voice/text) |
Yes (up to 50%) |
Choosing the right software depends on your practice size and billing needs. Smaller teams may prefer TheraBill or SimplePractice, while larger organizations might find Opus more effective for managing complex workflows.
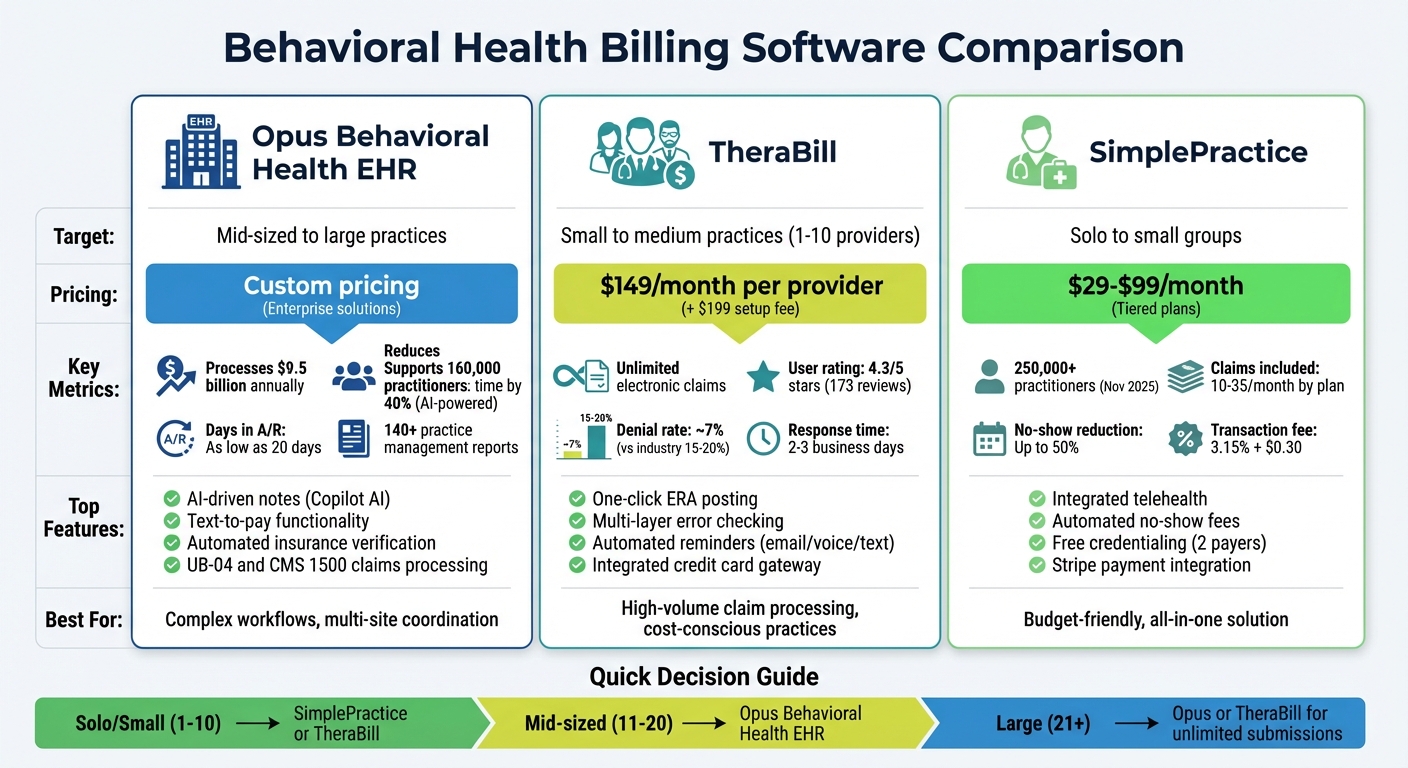
Behavioral Health Billing Software Comparison: Opus vs TheraBill vs SimplePractice
1. Opus Behavioral Health EHR
Revenue Optimization Features
The Opus Behavioral Health EHR system includes a Revenue Cycle Management (RCM) module that processes UB-04 and CMS 1500 claims, generating over $9.5 billion annually for private practices and supporting 160,000 practitioners daily[3].
A key feature is Copilot AI, an AI-powered scribe that drafts progress notes automatically, cutting documentation time by 40%. This allows clinicians to dedicate more time to patient care, which directly impacts revenue[3].
Other tools like automated insurance verification ensure coverage is confirmed before services begin, while intelligent lead routing captures new admissions, reducing the risk of revenue loss.
Additionally, payor rate compliance features help maintain accurate billing practices tailored to specific insurance requirements[3].
"With the ease of use for our clinical staff and clients, robust functionality for our back-office support, payor rate compliance features, and accrual accounting reporting... it was an easy choice." - Trevor Mulvey, VP of Finance, Care Counseling Clinics[3]
These tools work together to streamline revenue processes, making claim submissions more efficient and effective.
Claim Management Efficiency
Opus takes its revenue tools further with error reduction algorithms that scan clinical documents for mistakes before submission, minimizing denials.
This is particularly helpful for group sessions, where errors are more likely. For example, in February 2026, a mid-sized IOP facility in Texas reduced its 22% no-show rate to just 10% by using automated SMS reminders, recovering $1,500 weekly ($78,000 annually)[4].
The platform also features text-to-pay functionality, enabling patients or guarantors to pay co-pays and balances directly from their mobile devices.
This feature has significantly improved cash flow, reducing Days in A/R from the usual 60-day cycle to as few as 20 days[5].
Amanda Wilson, Director of Clinical Services at a mental health and substance use treatment center, shared:
"This process will simplify our operations to save so much time. We will no longer have to manually pull so many charts per quarter and have a timelier billing process for quicker reimbursements."[3]
Integration and Reporting Capabilities
Opus supports 140+ practice management reports, integrates lab services and e-prescribing into its workflow, and offers accrual accounting with real-time payment reconciliation[3][5].
Each transaction is logged with a full digital audit trail, including payer names, amounts, and timestamps, ensuring compliance and easy review during audits.
By combining these features, the platform provides a comprehensive solution for behavioral health practices.
2. TheraBill
After exploring Opus, let's take a closer look at TheraBill - a platform aimed at simplifying automation and reducing costs.
Revenue Optimization Features
TheraBill starts at $149 per provider, per month [6][7].
It emphasizes automation to minimize administrative tasks. One standout feature is its ERA functionality, which allows practices to post insurance and patient payments with just one click.
The platform also comes with an integrated credit card gateway, making it easy for patients to pay co-pays or settle outstanding balances. To further streamline operations, TheraBill sends automated appointment reminders via email and voice calls, with text reminders available for $0.10 per message [7].
Claim Management Efficiency
TheraBill allows unlimited electronic claim submissions to a wide network of payers, all without per-claim fees [8].
Its system uses multiple layers of error-checking to catch mistakes before claims are sent to insurers, with errors typically flagged within one to two days for quick corrections [8]. A Capterra user praised its efficiency, saying:
"It is top notch with the A/R and revenue portions. Posting payments, printing paper claims and account reconciliation are easy with this system." [7]
All claims are routed through established connections, eliminating the need for separate clearinghouse accounts [8][9].
For payers requiring paper submissions, TheraBill automatically generates CMS-1500 forms [8]. This robust error-checking process ensures smoother and more reliable claim submissions.
Scalability for Practice Sizes
TheraBill is best suited for solo practitioners and smaller group practices with fewer than 10 providers. Practices with 1–3 providers rate it 4.3/5, while larger teams with 16+ providers give it a lower 2.8/5 [7].
Although the platform allows unlimited non-provider logins for administrative staff, larger practices often encounter challenges with scheduling visualization and workflow management [7][9].
Customer service receives a 3.7/5 rating, with average response times of 2–3 business days [7]. Practices with more than 10 providers may need to carefully assess whether TheraBill's features can meet their growing demands.
Integration and Reporting Capabilities
TheraBill integrates seamlessly with WebPT and Google Calendar, although many users note that it operates primarily as a standalone system [7].
Its reporting tools include templates for claim aging, session balances, and nightly deposits, along with a custom report builder to analyze provider productivity and payer performance [9]. The Claim Aging Report is particularly useful for identifying unpaid claims before they exceed filing deadlines. Additionally, the platform stores a complete claim history in a digital filing cabinet, making audits more manageable [8].
Setup involves a one-time fee of $199, with data migration costs ranging from $500 to $1,500, depending on the size of the practice [6][7]. These features make TheraBill a solid choice for improving billing efficiency and managing revenue effectively.
3. SimplePractice
SimplePractice stands out as a billing platform tailored for behavioral health professionals.
Trusted by over 250,000 practitioners as of November 2025 [11], it offers a comprehensive suite of tools combining scheduling, documentation, and payment processing. Pricing begins at $29 per month for the Starter plan, $69 for Essential, and $99 for Plus [13].
These plans are designed to help practices streamline their operations and improve revenue management, as detailed below.
Revenue Optimization Features
SimplePractice integrates with Stripe for payment processing, applying a fee of 3.15% plus $0.30 per transaction [13]. To avoid disruptions, its Account Updater feature automatically refreshes expired or updated card details [16]. The platform also simplifies billing by automatically applying no-show fees, ensuring full session charges without the need for manual invoices [13]. Additionally, automated appointment reminders - sent via text, email, or voice - can significantly reduce no-show rates, reportedly by up to 50% [10]. For new users, SimplePractice offers free credentialing with up to two insurance payers, helping expand their billable network [10].
Claim Management Efficiency
The system is designed to streamline claims processing with tools like pre-submission validation, which flags claims missing critical details such as NPI, Tax ID, diagnosis codes, or member IDs [15].
Practices can submit claims individually or in batches using the "Unbilled Appointments" page, which allows filtering by payer or clinician [15].
The Essential plan includes 10 free claim submissions per month, while the Plus plan includes 35, with additional claims costing $0.25 each [13].
For added convenience, Electronic Remittance Advice (ERAs) automatically posts insurance payments and write-offs into the system [14]. For out-of-network clients, the platform generates and shares superbills through the client portal [14].
Scalability for Practice Sizes
SimplePractice caters to both solo practitioners and larger group practices. It offers role-based permissions and customizable access levels for schedulers, billers, and supervisors [12].
The Plus plan goes a step further by providing income allocation reports, which consolidate payment and appointment data to simplify payroll management for group practices [12].
However, group practices should note the additional cost of $59 per clinician per month [13]. The platform also supports complex NPI configurations, ensuring compliance with payer-specific requirements by populating both rendering provider and organization NPIs as needed [15].
Integration and Reporting Capabilities
A centralized analytics dashboard provides real-time insights into income, outstanding balances, and claim statuses.
All financial and clinical reports can be exported as Excel or CSV files for further analysis [11].
These tools enable practices to track referral sources that drive the most revenue and monitor unpaid insurance appointments to prevent revenue loss [11].
For psychiatrists and nurse practitioners, an ePrescribe add-on is available for $49 per month per clinician, plus a one-time $89 setup fee, allowing medication management within the same system [12].
Additionally, in 2024, SimplePractice introduced 19 new measurement-based care assessments, helping practitioners monitor client progress while managing billing operations [12].
Pros and Cons
Here’s a look at the strengths and limitations of each platform to help you make an informed decision.
Opus Behavioral Health EHR stands out for its ability to handle multi-site coordination and support various levels of care. This makes it a solid choice for mid-sized treatment centers dealing with complex billing workflows. Its integrated CRM and admissions tools help reduce manual data entry errors, streamlining clinical documentation. On the downside, it doesn’t offer native ERP features like property management or HR tracking, which might be essential for larger organizations [18].
TheraBill is tailored for high-volume claim processing, offering unlimited electronic claim submissions. With a 4.3 out of 5 stars rating from 173 users [17], it’s known for its pre-submission scrubbing feature, which identifies coding errors before claims are submitted. This can significantly lower denial rates - from the industry average of 15–20% to around 7% [1]. However, it falls short in providing 24/7 live customer support and has limited integration options [2].
SimplePractice is designed for solo practitioners and small groups, offering an easy-to-use interface and integrated telehealth features. Priced between $29 and $99 per month, it’s a budget-friendly option [18]. That said, it struggles with scalability, lacking features like residential treatment support, utilization review, per-diem billing, CRM, and advanced RCM capabilities [18].
To ensure your practice aligns its tools with revenue needs, consider calculating your denial rate by dividing non-accepted claims by total claims. When exploring systems during demos, check if the platform prevents scheduling beyond authorization limits rather than fixing errors after submission [2].
Conclusion
Selecting the right billing software largely depends on the size of your practice and the complexity of its operations.
For solo practitioners and smaller groups (1–10 clinicians), it’s often best to choose a budget-friendly platform with essential features like basic billing and telehealth tools. These practices typically focus on keeping costs low while ensuring smooth scheduling integration.
Mid-sized practices (11–20 clinicians) usually need a solution that connects clinical workflows with billing processes seamlessly. For example, Opus Behavioral Health EHR offers a user-friendly interface, built-in CRM, and strong revenue cycle management tools. These features help reduce manual errors and support efficient scaling.
Larger treatment centers (21+ clinicians) benefit most from software that includes unlimited electronic submissions and automated pre-submission scrubbing. These tools can cut denial rates from the industry average of 15–20% to around 7% [1]. Such organizations often require dedicated IT and billing teams to handle the complexities of payer-specific rules across multiple sites.
When evaluating vendors, test if the system proactively blocks scheduling errors, like exceeding authorization limits, rather than identifying them later in the billing process.
FAQs
How do I know if my billing software is causing claim denials?
To figure out if your billing software is causing claim denials, start by keeping an eye on your denial rates and digging into the specific denial codes. Patterns in these codes can point to recurring issues.
Also, check if your software offers features like real-time denial tracking and claim status updates. These tools can make it easier to spot problems early.
Common culprits behind denials include:
1.) Missing or incomplete patient information2.) Incorrect insurance coverage details
3.) Missing prior authorization for services
If these errors keep popping up, your software might be part of the problem. Fixing these issues can lead to fewer denials and better overall billing accuracy.
What features reduce days in A/R the fastest for behavioral health practices?
Behavioral health practices can speed up reimbursements and improve cash flow by leveraging tools like automated billing, claims scrubbing, and real-time benefits verification. Here's how these features make a difference:
Automated Billing: Simplifies the billing process, reducing manual errors and ensuring invoices are sent promptly.
Claims Scrubbing: Identifies and corrects potential issues in claims before submission, cutting down on denials and delays.
Real-Time Benefits Verification: Confirms patient coverage instantly, preventing billing surprises and speeding up approvals.By streamlining these processes, practices can minimize delays in payments and enhance overall financial efficiency.
What should I check in a demo to prevent authorization and coding errors?
When evaluating a demo of behavioral health billing software, look for features that simplify and streamline your billing process.
Key functionalities to prioritize include authorization tracking, which helps navigate complex requirements, and detailed documentation workflows to ensure accurate use of time-based billing codes like CPT 90837 and 90834.
Additionally, the software should offer claims scrubbing to catch errors before submission, denial management tools to handle rejected claims efficiently, and compliance tools to meet payer regulations.
Together, these features can reduce mistakes and make your billing process more efficient.
